Abstract
Background
Diabetes outcomes are worse for underserved patients from certain ethnic/racial minority populations. Telephonic disease management is a cost-effective strategy to deliver self-management services and possibly improve diabetes outcomes for such patients.
Objective
We conducted a trial to test the effectiveness of a supplemental telephonic disease management program compared to usual care alone for patients with diabetes cared for in a community health center.
Design
Randomized controlled trial.
Participants
All patients had type 2 diabetes, and the majority was Hispanic or African American. Most were urban-dwelling with low socioeconomic status, and nearly all had Medicaid or were uninsured.
Measurements
Clinical measures included glycemic control, blood pressure, lipid levels, and body mass index. Validated surveys were used to measure dietary habits and physical activity.
Results
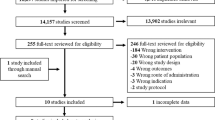
A total of 146 patients were randomized to the intervention and 149 to the control group. Depressive symptoms were highly prevalent in both groups. Using an intention to treat analysis, there were no significant differences in the primary outcome (HbA1c) between the intervention and control groups at 12 months. There were also no significant differences for secondary clinical or behavioral outcome measures including BMI, systolic or diastolic blood pressure, LDL cholesterol, smoking, or intake of fruits and vegetables, or physical activity.
Conclusions
A clinic-based telephonic disease management support for underserved patients with diabetes did not improve clinical or behavioral outcomes at 1 year as compared to patients receiving usual care alone.



Similar content being viewed by others
References
Mattke S, Seid M, Ma S. Evidence for the effect of disease management: is $1 billion a year a good investment? Am J Manag Care. 2007;13:670–676.
Norris SL, Nichols PJ, Caspersen CJ, Glasgow RE, Engelgau MM, Jack L, et al. The effectiveness of disease and case management for people with diabetes. A systematic review. Am J Prev Med. 2002;22:15–38.
Self-reported prevalence of diabetes among Hispanics-United States, 1994–1997. MMWR Morb Mortal Wkly Rep. 1999;48:8–12.
Diabetes among Hispanics-Los Angeles County, California, 2002–2003. MMWR Morb Mortal Wkly Rep. 2003;52:1152–55.
Centers for Disease Control and Prevention. National diabetes fact sheet: general information and national estimates of diabetes in the United States, 2005. 2005. Atlanta, GA, US Department of Health and Human Services, centers for Disease Control and Prevention. Ref Type: Report.
Ciechanowski PS, Katon WJ, Russo JE. Depression and diabetes: impact of depressive symptoms on adherence, function, and costs. Arch Intern Med. 2000;160:3278–85.
Gonzalez JS, Safren SA, Cagliero E, Wexler DJ, Delahanty L, Wittenberg E, et al. Depression, self-care, and medication adherence in type 2 diabetes: relationships across the full range of symptom severity. Diabetes Care. 2007;30:2222–27.
Lanting LC, Joung IM, Mackenbach JP, Lamberts SW, Bootsma AH. Ethnic differences in mortality, end-stage complications, and quality of care among diabetic patients: a review. Diabetes Care. 2005;28:2280–2288.
Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16:606–13.
Wakimoto P, Block G, Mandel S, Medina N. Development and reliability of brief dietary assessment tools for Hispanics. Prev Chronic Dis. 2006;3:A95.
Topolski TD, LoGerfo J, Patrick DL, Williams B, Walwick J, Patrick MB. The Rapid Assessment of Physical Activity (RAPA) among older adults. Prev Chronic Dis. 2006;3:A118.
Brown H, Prescott R. Applied Mixed Models in Medicine. Chicester, England: Jophn Wiley & Sons, Ltd; 1999. Ref Type: Generic.
Allison PD. Missing Data. University Papers Series on Quantitative Applications in the Social Sciences. Thousand Oaks, CA: Sage; 2001. Ref Type: Generic.
Rothman RL, Malone R, Bryant B, Shintani AK, Crigler B, Dewalt DA, et al. A randomized trial of a primary care-based disease management program to improve cardiovascular risk factors and glycated hemoglobin levels in patients with diabetes. Am J Med. 2005;118:276–84.
Taylor CB, Miller NH, Reilly KR, Greenwald G, Cunning D, Deeter A, et al. Evaluation of a nurse-care management system to improve outcomes in patients with complicated diabetes. Diabetes Care. 2003;26:1058–63.
Young RJ, Taylor J, Friede T, Hollis S, Mason JM, Lee P, et al. Pro-active call center treatment support (PACCTS) to improve glucose control in type 2 diabetes: a randomized controlled trial. Diabetes Care. 2005;28:278–82.
Peikes D, Chen A, Schore J, Brown R. Effects of care coordination on hospitalization, quality of care, and health care expenditures among Medicare beneficiaries: 15 randomized trials. JAMA. 2009;301:603–18.
de GM, Anderson R, Freedland KE, Clouse RE, Lustman PJ. Association of depression and diabetes complications: a meta-analysis. Psychosom Med. 2001;63:619–30.
Katon W, von KM, Ciechanowski P, Russo J, Lin E, Simon G, et al. Behavioral and clinical factors associated with depression among individuals with diabetes. Diabetes Care. 2004;27:914–20.
Lustman PJ, Anderson RJ, Freedland KE, de GM, Carney RM, Clouse RE. Depression and poor glycemic control: a meta-analytic review of the literature. Diabetes Care. 2000;23:934–42.
Chodosh J, Morton SC, Mojica W, Maglione M, Suttorp MJ, Hilton L, et al. Meta-analysis: chronic disease self-management programs for older adults. Ann Intern Med. 2005;143:427–38.
Lorig K, Ritter PL, Villa F, Piette JD. Spanish diabetes self-management with and without automated telephone reinforcement: two randomized trials. Diabetes Care. 2008;31:408–14.
Norris SL, Lau J, Smith SJ, Schmid CH, Engelgau MM. Self-management education for adults with type 2 diabetes: a meta-analysis of the effect on glycemic control. Diabetes Care. 2002;25:1159–71.
Anderson D, Christison-Lagay J. Diabetes self-management in a community health center: improving health behaviors and clinical outcomes for underserved patients. Clin Diabetes. 2008;26:22–27.
Gilmer TP, Philis-Tsimikas A, Walker C. Outcomes of Project Dulce: a culturally specific diabetes management program. Ann Pharmacother. 2005;39:817–22.
Glazier RH, Bajcar J, Kennie NR, Willson K. A systematic review of interventions to improve diabetes care in socially disadvantaged populations. Diabetes Care. 2006;29:1675–88.
Metghalchi S, Rivera M, Beeson L, Firek A, De LM, Balcazar H, et al. Improved clinical outcomes using a culturally sensitive diabetes education program in a Hispanic population. Diabetes Educ. 2008;34:698–706.
Peek ME, Cargill A, Huang ES. Diabetes health disparities: a systematic review of health care interventions. Med Care Res Rev. 2007;64:101S–56S.
Acknowledgements
Funding for this project was provided by a grant from the Connecticut Health Foundation.
Conflict of Interest
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Additional information
Funded by a grant from the Connecticut Health Foundation.
Rights and permissions
About this article
Cite this article
Anderson, D.R., Christison-Lagay, J., Villagra, V. et al. Managing the Space between Visits: A Randomized Trial of Disease Management for Diabetes in a Community Health Center. J GEN INTERN MED 25, 1116–1122 (2010). https://doi.org/10.1007/s11606-010-1419-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-010-1419-5