As some doctors tinker with their exclusively procured Google Glass devices, the medical community is being told to prepare for a future where life-saving information is available at a glance.
The device looks like a pair of eyeglasses without lenses and has a tiny computer and camera built into the frame. When users look up and to the right, they see a holographic screen that appears to be floating in front of them. Google Glass is operated through voice commands, head tilts and a touchpad on the side. It can take pictures, make video calls and enables hands-free web searching.
Some medical applications being explored include remote mentoring, viewing lab reports without looking away from patients and live streaming surgeries to medical students. Despite the buzz, however, there are constraints to medicine’s adoption of Google Glass, including privacy regulations and a reluctance among some hospital administrations to embrace new technologies.
In May, Google shipped 8000 devices to early adopters in the United States. Some of them are medical professionals, though Google spokesperson Aaron Brindle wasn’t able to say how many devices ended up in hospital settings.
Chris Madison, a simulation technician at Hartford Hospital in Connecticut, is among the early adopters. He is part of a pilot study in which a group of medical residents treats patient mannequins by reading monitors and checking lab results, while a second group has vital signs, medication, lab results and equipment malfunctions beamed to their wearable computers.
“The medical devices out there could potentially talk to this one system, and display all this information on Glass,” says Madison.
Other physicians are excited about how Glass could revolutionize medical education in areas such as surgery. “Students have to go to the operating room and peek behind your shoulder and try to see what you’re seeing in a small field,” explains Dr. Rafael Grossmann, a trauma surgeon at Eastern Maine Medical Center in Bangor. “With Glass, they get to see procedures from the surgeon’s perspective.”
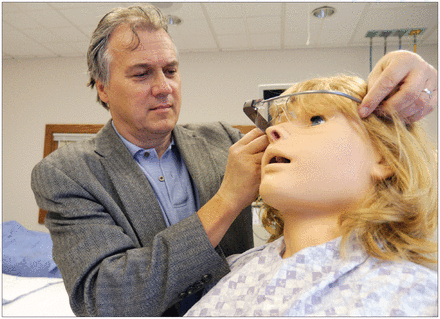
Some doctors think Google Glass could be a helpful educational tool when put on a patient or mannequin to allow residents to see from the patient’s perspective
Image courtesy of ETSU Photographic Services
The wearable camera is also a helpful educational tool when put on a patient or mannequin because it allows residents to view their bedside manner from the patient’s perspective, says Dr. Martin Olsen, the residency program director for obstetrics and gynecology at East Tennessee State University’s medical school in Johnson City. “The learner sees themselves and thinks, ‘I’d be a better doctor if I did x, y and z,’” says Olsen, who recently incorporated Glass into training.
Despite the early adopters’ excitement, however, it’s questionable whether many hospitals will make use of the James Bond–worthy technology. Dr. Steve Hawrylyshyn, a resident in family medicine at St. Michael’s Hospital in Toronto, Ontario, with a Master of Science degree in e-health, wrote in an email that Glass has “very neat and beneficial uses” but “even some of the more technologically advanced hospitals are still slow to digitalize.”
Another limit to incorporating Glass into health care is that medical devices are proprietary, adds Madison. Although it is feasible to integrate Glass with electronic medical records, which have centralized databases, the barriers are greater for machines like defibrillators, infusion pumps and heart monitors.
There are also technical shortcomings to be worked out — the battery life allows for only about 45 minutes of recording, for example.
A more important barrier may be hospital legislation. Currently, doctors can’t upload patient data onto Glass because that information is streamed through Google’s server, and the US Health Insurance Portability and Accountability Act does not allow a third party to access patient information.
“The technology is exponentially leaping forward at a pace that regulation is not keeping up with,” says Grossmann. “But it will happen. It will just take time.”











