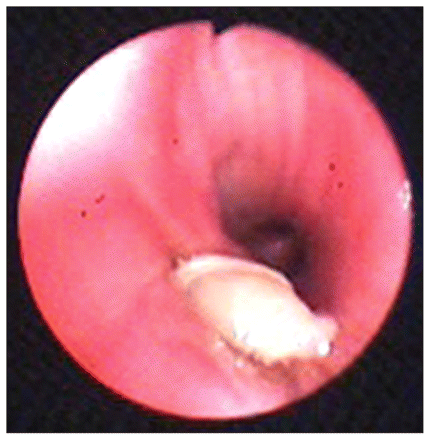
A 42-year-old previously healthy man presented to an outpatient clinic in India with a six-month history of cough, mucoid expectoration and hemoptysis. He had no history of fever or other constitutional symptoms. He was a nonsmoker and had no history of close contact with dogs or other animals. On examination, breath sounds were reduced in intensity over the right infrascapular area. A chest radiograph (Appendix 1A, available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.111185/-/DC1) and thoracic computed tomographic (CT) scan (Appendix 1B) did not lead to a clear diagnosis, but flexible bronchoscopy showed white gelatinous membrane-like structures protruding from the medial basal segment of the right lower lobe (Figure 1); Appendix 2, video available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.111185/-/DC1). A bronchoscopic biopsy confirmed these as characteristic laminated hydatid membranes (Appendix 1C). Hydatid serology was positive, and we diagnosed a ruptured pulmonary hydatid cyst. Abdominal ultrasonography was normal, with no evidence of hydatid cysts in his liver. Following surgical removal of the cyst (Appendix 1D), our patient had an uneventful recovery. He received oral albendazole preoperatively, and treatment was continued for three months.
(A) Flexible bronchoscopic image in a 42-year-old man with hemoptysis showing a white gelatinous membrane-like structure protruding from the medial basal segment of the right lower lobe.
Hydatid disease is an important public health problem in endemic countries. The disease is caused by the larval stage of Echinococcus granulosus, a tapeworm that affects dogs. Humans contract the disease by ingestion of eggs from contaminated water and food or from close contact with dogs. Pulmonary hydatid cysts are often asymptomatic and can be diagnosed incidentally on plain chest radiographs, but CT is the preferred imaging modality.1,2 With a sensitivity of only 50% in pulmonary echinococcosis, serologic tests can only support the diagnosis, which is primarily made on clinico-radiologic grounds.1,2 Surgical removal is the main therapeutic approach, and preoperative treatment with albendazole reduces the chances of parasite seeding and recurrence.1,2 Prolonged treatment with albendazole can reduce the size of pulmonary cysts that are not resected surgically.
When a cyst becomes infected or, as in our patient, ruptures, the clinico-radiologic profile can mimic diseases such as nonresolving pneumonia, tuberculosis, and abscess or tumour of the lungs. Direct bronchoscopic visualization with biopsy allowed us to quickly clarify the diagnosis, leading to our patient’s timely and effective treatment.3
See the following video online:
Appendix 2: Video of flexible bronchoscopy.
Footnotes
-
Competing interests: None declared.
-
This article has been peer reviewed.