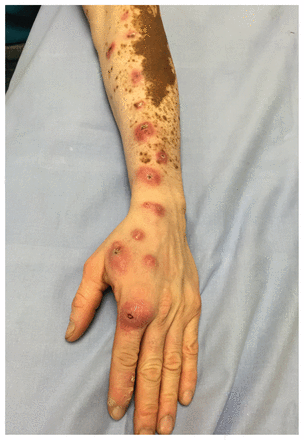
An immunocompetent 52-year-old man presented with lesions and inflammation on his left arm after lacerating his index finger while cleaning a fish tank (Figure 1). The lesions appeared at the laceration site two weeks after the injury and continued to progress for five months. He had no fever or systemic symptoms. On examination, erythematous and ulcerative papulonodules spanned from his left index finger to his upper arm in a sporotrichoid pattern. Laboratory results were normal, including negative bacterial, fungal and mycobacterial tissue cultures (at 30°C and 37°C). Skin biopsy showed dermal granulomatous inflammation with multinucleate giant cells, lymphocytes, histiocytes and plasma cells, although direct smears of tissue and special stains for fungi and acid-fast bacilli were negative. Based on the exposure, morphology and histopathology, we diagnosed Mycobacterium marinum infection. Treatment with doxycycline, 100 mg orally twice daily for three months, gave an excellent initial response. Subsequently, the patient was lost to follow-up.
Erythematous and ulcerative papulonodules spanning the left arm in sporotrichoid pattern and diagnosed as Mycobacterium marinum infection in a 52-year-old man after lacerating his left index finger while cleaning a fish tank.
M. marinum is a water-borne pathogen common in both fresh and saltwater fish.1 Infection typically occurs on the upper limbs several weeks after injury in aquatic environments or after handling fish.1–3 Although lesions are initially solitary or multiple, a linear distribution of papulonodular lesions along lymphatic channels resembling sporotrichosis can occur. The differential diagnosis also includes nocardiosis, leishmaniasis and other mycobacterial or fungal infections.2 Results of microbiologic studies are sometimes negative. One case series (n = 29) reported positive M. marinum cultures in 41% of probable infections.3 When the results of culture are negative, immunohistochemistry and polymerase chain reaction for mycobacterial 16S rRNA can be helpful.2 Systemic symptoms are rare, but deep infections such as septic arthritis and tenosynovitis can occur that require surgical intervention.3 Antibiotic treatment alone appears effective in 68%–100% of most noninvasive infections. 3 It typically includes single- or double-agent coverage with tetracyclines, sulfamethoxazole–trimethoprim, clarithromycin, ethambutol or rifampin for at least three to four months.1–3
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.