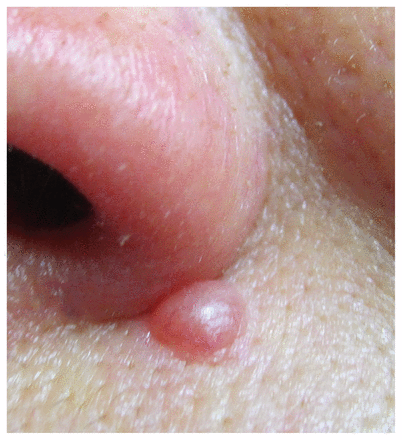
A 48-year-old woman presented with a papule of the left alar groove (Figure 1) that had been growing slowly for about two years. Clinical features (telangiectatic surface) suggested nodular basal cell carcinoma. Physical examination was otherwise normal.
Wiesner nevus on the left alar groove of a 48-year-old woman.
Histopathologic examination showed a dome-shaped neoplasm, with dermal nests infiltrated by lymphocytes comprising epithelioid cells showing oval- to kidney-shaped nuclei and abundant eosinophilic, often inclusionlike, cytoplasms. There were no atypical features (i.e., large sheets of cells, perineural/perivascular/periadnexal involvement, confluent pleomorphism, mitoses). Neoplastic cells showed loss of the constitutive nuclear immunostaining for BAP1 protein and were positive for the VE1 (anti-BRAFV600E mutated protein) antibody (Appendix 1, available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.160049/-/DC1). All these features were consistent with a Wiesner nevus.
Biallelic inactivating mutations of the BAP1 tumour suppressor gene on chromosome 3p21.1 and loss of nuclear immunoreactivity for the BAP1 protein are characteristic of BAPomas,1 which represent 0.005% of all excised melanocytic tumours. These range from completely benign (e.g., Wiesner nevus),2 as in this patient, to melanocytic borderline atypical intradermal tumours3 and to overtly malignant tumours. A BRAFV600E mutation, detectable with the VE1 immunostain, is present in about 70% of BAPomas.3
Wiesner nevus grows slowly, and no further action is necessary after excision of the nevus. However, the patient should be checked for the presence of multiple fibroma-like nevi. These nevi are the hallmarks of the uncommon familial tumour predisposition syndrome (Online Mendelian Inheritance in Man; OMIM:614327) caused by germline BAP1 inactivating mutations, which is associated with atypical Spitz tumours/melanocytic borderline atypical intradermal tumours, cutaneous and uveal melanoma, and internal neoplasms (e.g., mesothelioma, renal clear cell carcinoma, lung adenocarcinoma, squamous cell carcinoma of the head and neck, breast carcinoma, myelodysplasia, medulloblastoma and meningioma).1,3
Any cutaneous papulonodular lesion reported to be growing should be excised. If Wiesner nevus is diagnosed histopathologically and is associated with multiple cutaneous (fibroma-like) melanocytic tumours, the patient should receive genetic testing for tumour predisposition syndrome.
Acknowledgement
The authors thank Dr. Thomas Wiesner for his suggestions during manuscript preparation.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.