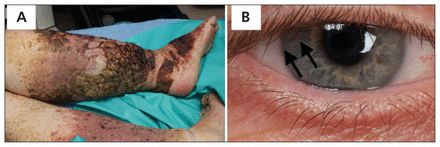
A 54-year-old man presented to the emergency department with bilateral swelling in his legs that was progressive, long-standing and had started when the patient was in his midthirties. Hyperkeratotic plaques and fissuring to midshin level on both legs also were observed (Figure 1A). He was otherwise healthy, with normal levels for liver enzymes and serum creatinine, and a negative result for protein on 24-hour urinalysis. Distichiasis (i.e., abnormal growth of eyelashes from the meibomian glands) was visible on closer physical examination of his eyelids (Figure 1B). Lymphedema-distichiasis syndrome was diagnosed, and his legs responded well to bathing and débridement.
(A) Bilateral lymphedema in the legs associated with hyperkeratotic plaques and fissuring to midshin level. (B) Patient’s right eye showing a second layer of eyelashes arising from the meibomian glands and directed toward the cornea (arrows).
The patient’s two brothers, grandmother and a maternal uncle also had lymphedema. Both brothers were in their late twenties when the condition developed, but no information was available for his uncle and grandmother. There was no reported family history of distichiasis, and genetic testing was unavailable.
Most cases of lymphedema are secondary and have infectious or iatrogenic causes. Primary lymphedema occurs in 1–3 out of every 10 000 live births,1 with a differential diagnosis that includes Milroy disease, lymphedema-distichiasis syndrome and hypotrichosis-lymphedema-telangiectasia syndrome. Primary lymphedema can also be a feature of certain inherited chromosomal conditions, such as Aagenaes syndrome, Noonan syndrome, Klinefelter syndrome, Turner syndrome, and trisomy 13, 18, 21 and 22.2
Lymphedema-distichiasis syndrome is a congenital lymphedema associated with the presence of aberrant eyelashes arising from the meibomian glands.3,4 It is a clinical diagnosis and can be associated with mutations in the FOXC2 gene;3 inheritance is autosomal dominant with variable penetrance.4 Bilateral lymphedema of the legs is usually present in the patient by age 30 years. Distichiasis is usually present at birth and can cause corneal irritation or recurrent conjunctivitis5 in up to 75% of patients; however, it was asymptomatic in this patient.
Clinical images are chosen because they are particularly intriguing, classic or dramatic. Submissions of clear, appropriately labelled high-resolution images must be accompanied by a figure caption and the patient’s written consent for publication. A brief explanation (250 words maximum) of the educational significance of the images with minimal references is required.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.