Osteoarthritis is a leading cause of pain, disability and health care use among adults. The hip is the second most common large joint affected by osteoarthritis.1–3 Although research has advanced our knowledge of osteoarthritis, no therapies currently exist that halt progression of the disease. In many cases, the disease progresses to damage and destruction of the joint. Consequently, orthopedic surgery has a critical role in the management of osteoarthritis.
More than 30 000 hospital admissions for hip replacement and revision surgery were reported across Canada in 2008/09, a 63% 10-year increase.4 Aging of the population; increased longevity, arthritis prevalence and rates of obesity; and expanding indications for hip surgery portend a continuing upward trend in demand for surgical management of hip osteoarthritis.
Although there have been many advances in surgical techniques and approaches for hip osteoarthritis, debate continues on the optimal management for the individual patient. In this review, we discuss indications for surgery, review surgical approaches and component materials, and suggest future directions. We reviewed randomized clinical trials, meta-analyses, and prognostic, observational and retrospective studies (Box 1).
Summary of literature review
We performed a literature search of PubMed (1980 to January 2013), Embase (1980 to January 2013) and MEDLINE (1950 to January 2013) databases. We used a combination of Medical Subject Headings, including “hip replacement,” “hip arthroplasty,” “hip resurfacing,” “metal-on-metal,” “ceramic hip,” “minimally invasive hip surgery,” “mini-incision hip surgery,” “hip replacement outcomes,” “metal-on-polyethylene hip replacement,” “revision hip replacement” and “meta-analysis.” Reference lists of selected articles were also reviewed for additional studies. Two of us abstracted and reviewed all data. We included the best evidence, including clinical trials, meta-analyses, prognostic studies, observational studies and retrospective studies, as available.
When should patients be referred for surgical assessment?
Referral for surgical assessment should be considered for patients who experience hip symptoms (e.g., pain, restricted function and stiffness) that substantially affect quality of life and are unresponsive to pharmacologic and nonpharmacologic treatments.5–7 Evidence suggests that early referral, before extensive functional limitation and pain, and early intervention are associated with better patient-reported pain and function following surgery (Table 1).8–15
Associations between early referral and postsurgical outcomes
Although patient-specific factors, including age, sex, obesity and comorbidities, may variably influence patient-reported outcomes after surgery (Table 2),16–18 there is no suggestion that these factors should be barriers to referral, and these factors are not used for wait-list prioritization. Even if certain subgroups fare less well after joint replacement, this does not mean that, on average, they do not receive benefit.18 Further, there is no consensus on the use of scoring tools or algorithms by which referral is based on a specific threshold being reached.
Patient-specific factors as predictors of patient-reported outcomes following total hip replacement
Glycemic control is critical because diabetes confers an increased risk of deep infection (relative risk 2.11, 95% confidence interval [CI] 1.41 to 3.17) after surgery.19 Also, cessation of smoking for 6–8 weeks before intervention has been shown to decrease wound complications (absolute risk reduction of 26%).20 Among patients taking newer-generation antiplatelet agents such as clopidogrel, it is recommended that these medications be stopped 7 days before surgery, particularly if spinal or epidural anesthesia is being considered.21 Finally, hip replacement should be delayed 1 year after cardiac stent placement.22 Individual risk–benefit evaluation is essential.21,22
What surgical options are there?
In the early stages of osteoarthritis, joint-preserving procedures such as pelvic osteotomy (for insufficient acetabular coverage of the femur) or hip arthroscopy (for femoroacetabular impingement) may be considered depending on the patient’s underlying diagnosis. These procedures are generally not recommended for patients with advanced degenerative changes. Patients with advanced joint damage are best referred to a surgeon to consider the options of either hip resurfacing or total hip replacement.
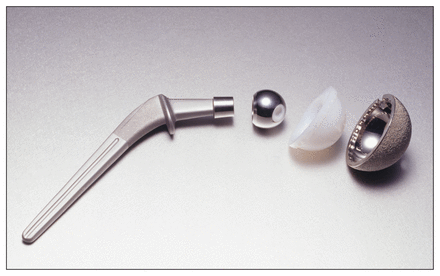
In a traditional hip replacement, the femoral head and damaged acetabulum are both removed and replaced with metal, plastic or ceramic components (Figure 1). Cement may be used for fixation, but most hip replacements performed in Canada are now uncemented23 owing to longer implant survival.24–26 Although ethical concerns, and costs, preclude clinical trials for establishing the merits of hip replacement,27 many observational studies have shown this procedure to be highly effective (and cost-effective) in minimizing pain and restoring function.16,28–34 Because surgical techniques and the design of prostheses and materials have improved over several decades, the risks of complications and early revisions following replacement have diminished. Rates of complications occurring within 90 days after surgery were found to be 1.0% for mortality, 0.9% for pulmonary embolus, 0.2% for wound infection, 4.6% for hospital readmission and 3.1% for hip dislocation among the US Medicare population.35 Ten-year revision rates after surgery can range from 5% to 20%, depending on age and fixation technique.36
Components of traditional hip replacement.
Image courtesy of Photodisc/Thinkstock
Despite the overall success of hip replacement, studies have documented that 5% to 25% of patients who undergo this procedure report minimal improvement or dissatisfaction with their outcomes.14,16–18,37–43
In hip resurfacing, the femoral head is left in place but trimmed and capped with a metal covering. The damaged acetabulum cartilage is removed and replaced with a metal shell, similar to a traditional hip replacement. The proposed advantages of resurfacing include bone conservation among patients likely to outlive a traditional replacement (i.e., younger patients), improved hip range of motion and the potential for allowing younger patients an increased level of activity. Reported disadvantages include increased risk of femoral neck fracture, more bone loss on the acetabular side, a more difficult operation requiring larger incisions, and increased risk of systemic exposure to metal ions resulting from wear of the metal-on-metal bearing surface.44–49
Hip resurfacing is predominantly considered for the young active patient with end-stage osteoarthritis.47 Early and mid-term follow-up generally has shown comparable results to those of standard replacement.50–59 However, complications particular to this procedure have been identified (as stated previously), and emphasis is placed on patient selection, component selection and surgical technique to avoid poor and adverse outcomes and short-term failures.44,47,60–70 Many surgeons avoid resurfacing in postmenopausal women because of an increased risk of femoral neck fracture, and in those with known renal insufficiency owing to the potential for metal ion accumulation.
Earlier generations of resurfacing devices frequently failed, often because of problems with excessive wear of the bearing surface materials. Since then, improvements in surgical technique and design have led to a renewed interest and use of hip resurfacing.
Is hip replacement or is hip resurfacing the best approach?
Matched comparative studies and clinical trials have compared short- and long-term outcomes of hip resurfacing versus hip replacement (Table 3).48,56,58,70–73 One of the larger matched studies with 5-year follow-up compared patients who had undergone hip resurfacing with those who had undergone traditional hip replacement.56 The authors found that the hip resurfacing group were more active in running (58.5% v. 13.7%, p < 0.001), sports (73.6% v. 33.3%, p < 0.001) and manual labour (60.4% v. 39.2%, p = 0.049).56
Selected studies comparing outcomes of total hip replacement and hip resurfacing
The consensus from 3 clinical trials70,71,74 is that hip resurfacing has no added advantage with respect to gait speed, stride length, stair climbing,71 range of motion74 or health-related quality of life.70,71,74 One study found that a substantially higher number of patients who had undergone hip resurfacing returned to moderate or high activity levels 1 year after surgery (77%) compared with those who had undergone hip replacement (39%).75 No published trial appears to be adequately powered to compare the complication rates of resurfacing versus replacement, however.
Limited to short-term follow-up, current trial evidence does not adequately address the difference in implant lifespan between resurfacing and replacement. Norwegian73 and Australian72 registry data showed increased rates of revision at 2 and 5 years, respectively, for resurfacing versus replacement. Longer-term follow-up periods for present resurfacing designs are needed. A recent UK-based registry study reported high revision rates among women who had undergone hip resurfacing (8.5% at 5 yr), and the authors advocated against resurfacing in female patients.48
Given the added expense of implants used in hip resurfacing, a cost–benefit analysis should be considered in future trials comparing this procedure with hip replacement.
Is mini-incision hip surgery preferable to conventional hip surgery?
The traditional approaches to hip replacement are the direct lateral and posterior approaches. The traditional incision is typically 15 cm or greater in length. Differences have not been shown for dislocation, limp or function between the 2 approaches.76 Mini-incision hip surgery was developed with the goal of decreasing tissue injury and blood loss, and improving patient outcomes. Although there is no universally accepted definition of mini-incision, many define it as an incision less than 12 cm in length. Patients considered appropriate candidates should have a body mass index of 30 or less, or a thigh circumference of less than 50 cm.77,78 Clinical trial evidence comparing mini-incision with conventional approaches is limited (Table 477,79,80). For smaller incisions, findings suggest no difference for in-hospital morphine use (mean 42.9 ± 97.4 mg v. 45.0 ± 96.8 mg, p = 0.89), and reduced intraoperative blood loss (mean 314 ± 162 mL v. 366 ± 190 mL, p = 0.03) but no difference in transfusion rates (mean 0.42 ± 0.95 units v. 0.30 ± 0.66 units, p = 0.27).77,79,80 Differences in patient function 3 months and 1 year after surgery were not found.80,81
Selected studies comparing outcomes of minimally invasive and standard-incision total hip replacement
What are the comparative benefits and risks of metal-on-metal versus other bearing surfaces?
Metal-on-metal and other “hard-on-hard” bearing surfaces such as ceramic have gained popularity in recent decades because of their potential for less wear and improved implant longevity over traditional polyethylene bearing surfaces. To date, trial evidence has not indicated any benefit of hard-on-hard bearing surfaces over polyethylene for implant survivorship (Table 5).82–88 A recent UK-based registry report showed higher revision rates for metal-on-metal bearing surfaces (6.57%, 95% CI 5.10% to 8.43%) compared with ceramic (3.00%, 95% CI 2.45% to 3.68%) and polyethylene (2.03%, 95% CI 1.69% to 2.44%) at 7-year follow-up.89 The concern with metal-on-metal implants is the accumulation of cobalt and chromium ions in the body, with a potential for cardiac toxicity, local soft-tissue erosions (pseudotumours, estimated incidence of 1% at 5 yr90) or neurologic complications.45,91–93 A case series that reported on early failures (within 2–3 yr of surgery) cited implant loosening in 56% of these failures, and the remainder as soft-tissue reactions, pseudotumours and persistent pain.94 These implants have recently garnered substantial media attention owing to some companies removing their products from the market over concerns of early failures, and owing to safety advisories from the US Food and Drug Administration and Health Canada.95,96 Metal-on-metal bearings should be avoided in women of child-bearing age because of the risk of metal ion accumulation. Patients with metal-on-metal hip replacements without symptoms should have regular follow-up by their surgeon.
Selected studies comparing outcomes of metal-on-metal and metal-on-polyethylene hip replacement
Ceramic implants have not shown improved longevity over polyethylene, and they have the potential risk of fracture.97 Further, up to 10% of ceramic hips may have an audible “squeak,” which is troubling enough that patients have required revision to change the bearing surface.98 Clinical trial data and cost–benefit analyses, with a minimum 15–20 years of follow-up, are still needed to definitively address the issue of “best” bearing surface.
What management options exist when patients require revision?
Based on expert consensus, patients with implants should be followed biennially by an orthopedic surgeon, regardless of symptoms, for clinical and radiologic investigation of implant wear. Symptoms of implant wear or loosening may include groin or thigh pain, or symptoms of hip instability (i.e., a feeling of giving way).
Revision surgery, including multiple revisions, may be required for a diagnosis of aseptic loosening of 1 or both components, recurrent dislocation or infection. For recurrent dislocation, assuming adequate component alignment, the surgical options are revision to a larger femoral head or a hip-stabilizing (constrained) acetabular component. For aseptic loosening, revision options exist; however, bone grafting, cement or metallic augments may be needed to compensate for bony defects. For infection, the common procedure is a 2-stage revision, whereby the components are removed and a temporary implant is used to deliver local antibiotic therapy in addition to parenteral antibiotic therapy. Following infection eradication, new hip implants are inserted. Length of stay in acute care after revision is generally longer than for the primary operation (6.2 v. 4.0 d), and patients report worse pain and poorer function at 5 years following revision compared with the primary surgery.99,100
Future directions
More people are living longer and indications for hip surgery are expanding to include younger patients, which suggest a potentially greater future demand for revision surgery. To minimize this likelihood, continued improvement of design, materials and surgical techniques are key.101
As indicated, there are still gaps in our understanding of the benefits and disadvantages of hip resurfacing versus hip replacement, mini-incision versus conventional approaches, and optimal bearing surfaces. These areas require further research.
Efforts in tissue engineering and biologic therapies for osteoarthritis have focused on repair of cartilage defects. Methods have included bone marrow stimulation techniques, osteochondral grafting and chondrocyte implantation.102,103 Although many are investigating stem cell use in cartilage regeneration, limited evidence is currently available to support routine use of this technique.
Key pointsTotal hip replacement with a metal-on-polyethylene bearing surface remains the gold standard for the treatment of end-stage hip osteoarthritis, providing reliable improvement in pain and function with consistent implant longevity.
Registry reports suggest an increased rate of revision for hip resurfacing compared with total hip replacement, particularly among female patients.
A further registry report showed an increased failure rate of metal-on-metal bearing surfaces compared with ceramic and polyethylene at 7 years.
The outcomes of revision total hip replacement are poorer than those of primary replacement, with patients reporting worse pain and poorer function at 5 years after revision surgery.
Footnotes
Competing interests: Rajiv Gandhi has received speaker fees from Smith & Nephew and conducted research funded by Bayer. Nizar Mahomed has received speaker fees from Smith & Nephew, and his institution has received research funds from Smith & Nephew and Biomet. No competing interests declared by Anthony Perruccio.
This article has been peer reviewed.
Contributors: All of the authors contributed to the conception and design, and drafting and revision of the article, and approved the final version submitted for publication.