- © 2008 Canadian Medical Association
As a general rule of thumb, if you'd like better odds of surviving a visit to a Canadian hospital, hope that you are hospitalized in New Brunswick, Saskatchewan, Alberta or British Columbia.
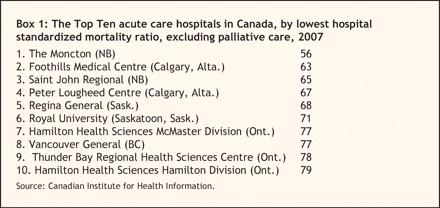
Hope also that it's the Moncton, Calgary Foothills, Saint John Regional, Calgary Peter Lougheed or Regina General hospitals, or in a pinch, the Saskatoon Royal University, Hamilton McMaster or Vancouver General (Box 1).
Conversely, hope your hospital isn't in Newfoundland and Labrador, Manitoba or Ontario, and, in particular, that it isn't the Kitchener Grand River, St. Catharines Niagara or pretty much any hospital in Scarborough.
However fair or valid, such are the conclusions that will inevitably be drawn by Canadians accessing the newly minted hospital standardized mortality ratio report from the Canadian Institute for Health Information (CIHI).
The quality indicator is essentially a measure of the number of “observed” to “expected” deaths within a hospital or health region for diseases or conditions that account for 80% of in-patient mortality in Canada, after adjusting for such factors as age, sex, diagnoses, length of stay, admission status, comorbidities and whether a patient was transferred from another institution.
In Canada, some 65 diagnosis groups cause 80% of in-hospital deaths, led by acute myocardial infarction, heart failure, pneumonia, chronic obstructive pulmonary disease, septicemia, malignant neoplasm of bronchus or lung, stroke, cerebral infarction, respiratory failure and hip fracture. In that context, hospital standardized mortality ratios are thus unique to a nation, in large measure because they reflect local diagnosis groups. Gun shot wounds, for example, do not make the cut in Canada but are a leading cause of death in the United States.
In turn, the findings generate an “odds ratio” of dying in hospital, or an estimated increase in risk for various predictors. Each additional year of age, for example, adds a 5% risk of dying. An emergency, rather than a planned, admission, increases the odds by 160%. Men have a 9% higher chance of dying. Patients transferred from another acute care facility: 35%. Patients with 2 comorbidities on the Charlson index: 95%. With 3: 244%. As for length of stay, relative to a 3–9-day stay, someone hospitalized 1 day has a 270% increased risk of dying. It's 80% for 2 days, 1% for 10–15, 17% for 16–21 and 53% for more than 21.
CIHI reported hospital mortality ratios only for health regions that had at least 2500 qualifying deaths between April 2004 and March 2007. Essentially, that threshold precluded the inclusion of Prince Edward Island or any territories. Quebec was not included because of “historical differences in the diagnosis and intervention classification systems,” says Institute Vice-President, Research and Analysis, Jennifer Zellmer.
As well, because of variations in how hospitals report and handle palliative care patients, mortality ratios were generated in 2 categories: excluding and including palliative care patients.
The mortality measure was developed in Great Britain as a predictor for variations in mortality rates among hospitals and it was concluded the biggest factors were emergency admissions, number of doctors per bed and number of general practitioners per capita in the hospital's locality. When used in the United States, factors accounting for variations included the payer (e.g., Medicare), hospital admission rates and the number of discharges to nursing homes or other health care facilities.
In Canada, though, CIHI and health care administrators say the ratio should be viewed as a “driver” of change or progress through time, rather than as a measure of hospital performance.
“The key here is to focus on your trend over time, not compare yourself to others,” Zellmer says, adding that such comparisons aren't valid because of such factors as differences in the way hospitals chart and code deaths or things like under-or over-coding of comorbidities.
The Canadian version has been under development for over 3 years and the process has already had a beneficial effect, as the national ratio dropped 5.6% from 2004/05 to 2006/07, said Institute President Glenda Yates at a press conference at which the ratios were unveiled.
Canadian Patient Safety Institute Chief Executive Officer Phil Hassen argues that there is still considerable room for improvement, given than an estimated 9000–23 000 deaths annually in Canada are a function of adverse events and a significant portion of those are occurring in hospitals. “It's hard to attribute anything to anything, but it's such a macro number, I assume that within those deaths are many that are the product of adverse events.”
Hassen had earlier told reporters that the ratios were strictly a measure of preventable deaths, with 100 being “the average number of people dying from adverse events.” But Zellmer says they should not be directly viewed as a measure of preventable death as the links between mortality and process or quality of care have not been conclusively established. “The notion of preventable is not black and white.”
The report indicates that in the first year of calculations, there were 37 acute care hospitals across the country with ratios under 100. By 2006/07, that had grown to 48. In 2004/05, there was a hospital (Grand River) with a staggering 158 ratio. That has since declined to 136.
From that perspective, a high hospital standardized mortality ratio should be viewed as “kind of red flag or an indicator” that a hospital needs to move with programs or measures to improve patient safety, says Sharon Sholzberg-Grey, president of the Canadian Healthcare Association (formerly known as the Canadian Hospital Association).
Ontario Hospital Association President Hilary Short concurs, arguing that the ratios are a “tool for performance improvement,” not a verdict on individual hospitals or health regions. “It's not the whole story and it should not be.”
The mortality indicator is now being used in the United Kingdom, United States, Netherlands and Sweden and “the experience has shown that there are ways to use this tool as a constructive measure,” Short adds.
Among measures that hospitals have used to reduce ratios are ones like the introduction of rapid response teams, medication reconciliation, infection control, standardization of wound and skin care, chart audits or the use of an intervention called a “VAP bundle” to prevent ventilator-assisted pneumonia.