The Case: A 70-year-old man presented with a 3-day history of abdominal cramping, nonbloody diarrhea and fever. The patient had returned 2 weeks earlier from a trip to a 5-star all-inclusive resort in Punta Cana, Dominican Republic, where he had eaten food only at the resort and had drunk bottled water. He had made no day trips. In the final days of his trip, the patient had developed watery diarrhea that resolved spontaneously shortly after he returned to Canada. He had not received pretravel vaccinations, nor had he taken malaria prophylaxis. The patient's medical history included gastritis that had been treated with pantoprazole and successful catheter ablation for treatment of atrial fibrillation.
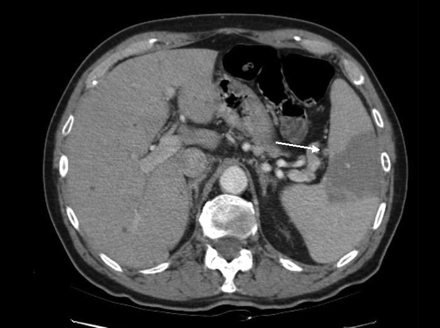
On physical examination, the patient was free of symptoms of severe infection with a temperature of 39.0°C, heart rate 82 beats/min and regular, and a blood pressure of 124/77 mm Hg. He had right lower-quadrant abdominal pain without signs of peritonitis. There was no rash. The results of routine blood tests were normal. A CT scan showed thickening of the ileocecal valve with adjacent mesenteric adenopathy. A thrombus in the splenic artery and splenic hypodensity were seen, consistent with infarction (Figure 1). A colonoscopy revealed patchy ulceration from the sigmoid to terminal ileum; biopsy showed nonspecific inflammation and ulceration. Blood, urine and stool cultures were obtained before initiation of ciprofloxacin (500 mg twice per day) and metronidazole (500 mg three times per day). The cultures were negative; however, the patient's fever and abdominal symptoms resolved. He was discharged home to complete a 14-day course of antibiotics.
Figure 1: A CT scan showing a thrombus in the splenic artery and splenic hypodensity.
Twelve days after discharge from hospital, the patient was readmitted with intermittent atrial fibrillation coinciding with a fluctuating fever. The patient reported that his fever had recurred 2 days after the antibiotic course was completed. A repeat CT scan showed resolution of the ileitis; however, a large fluid collection had formed in the spleen, consistent with a hematoma.
A consultation with an infectious disease specialist was requested several days later. The working differential diagnosis included malaria and organisms responsible for mesenteric adenitis (Box 1), infected splenic hematoma or abscess, and other causes of fever and diarrhea in a returning traveller (i.e., protozoan and helminthic infections). Repeat cultures of the patient's stool, blood, urine and bone marrow were negative, as were the results of the appropriate serologic tests. The results of 3 blood smears for malarial parasites were negative, as was the stool for ova and parasites. During readmission, the patient appeared well with sporadic fever despite not receiving antibiotic therapy.
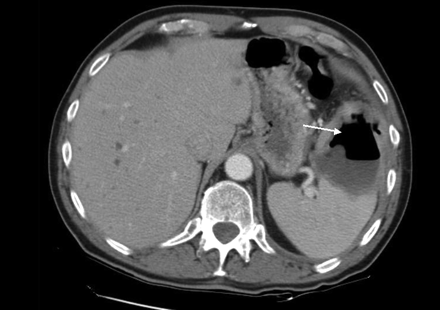
A follow-up CT scan performed 12 days after readmission revealed a new air pocket within the splenic hematoma (Figure 2). Culture of aspirated fluid revealed the presence of Salmonella enteritica serovar Typhi. Antimicrobial sensitivity testing showed resistance to nalidixic acid and sensitivity to ciprofloxacin, ampicillin, trimethoprim-sulfamethoxazole, chloramphenicol and third-generation cephalosporins. A splenic drain was performed and the patient received 4 weeks of ceftriaxone (1 g/day) therapy. He remains asymptomatic over 1 year after completion of therapy.
Figure 2: A follow-up CT scan obtained 12 days after readmission showing a new air pocket within the splenic hematoma.
This case highlights a number of important issues about typhoid fever, including the elusiveness of a diagnosis and the ever-changing demographics and resistance profiles. Historically, typhoid fever is associated with poor hygiene and sanitation, and it continues to cause significant morbidity and mortality worldwide. Humans are the only reservoir of infection; ingestion of food or water contaminated with feces is the predominant mode of transmission.
Within hours of ingesting the bacteria, the patient may develop self-limiting diarrhea corresponding to penetration of the bacteria into the intestinal mucosa and the underlying lymphoid tissues. After an asymptomatic incubation period of 10–14 days, a fever develops along with an array of systemic symptoms, particularly those affecting the gastrointestinal and central nervous systems. Diarrhea and constipation are equally common and are usually accompanied by nausea and anorexia. Headaches are common, and confusion and seizures may occur in more severe cases. Typhoid fever is known to have widespread complications that can occur at any time during bacteremia.1 Classic features such as relative bradycardia and salmon-coloured maculopapular lesions (rose spots) are present in less than 50% of cases.2
Gastrointestinal lymphoid and mucosal ulceration and necrosis occur in most cases and tend to cluster around the ileocecal valve. Inflammation of the mesenteric lymph nodes predominantly in the right lower quadrant is referred to as mesenteric adenitis. There are multiple infectious causes of mesenteric adenitis (Box 1), which may be confused with acute appendicitis. If left untreated for several weeks, inflammation caused by typhoid fever may lead to intestinal hemorrhage and perforation.
S. typhi can be cultured from various sites, including blood, stool, urine and rose spots. A feature unique to typhoid fever is that bone marrow cultures typically have the highest probability of a positive culture, with a sensitivity of 80%–95%.1,2 Unlike cultures from other sites, the yield from bone marrow is not reduced after several days of antibiotic therapy.2 Importantly, cultures from blood and stool are positive in only 70% and 30% of cases respectively.2
Fluorquinolones are considered the most effective therapy for drug-susceptible typhoid fever (Box 2). With this type of therapy, fever typically resolves within 4 days, with a cure rate of up to 98% and a chronic carriage rate of less than 2%.1,2 However, antimicrobial resistance has become a global issue in the treatment of typhoid fever. Multidrug-resistant typhoid strains (resistant to ampicillin, trimethoprim-sulfamethoxazole and chloramphenicol) have been identified worldwide. In the last 10 years, quinolone resistance has become problematic. Direct testing for susceptibility to ciprofloxacin and other higher generation quinolones is not reliable. Instead, nalidixic acid, a first-generation quinolone, is recommended as a surrogate marker of drug susceptibility. The failure of quinolone for treatment of typhoid strains resistant to nalidixic acid is well known.1–3
Although prevalent in parts of Africa and Asia, isolates that are resistant to nalidixic acid are not typical in North and South America. First-line therapy remains fluoroquinolones, particularly if the isolate is not resistant to nalidixic acid. Azithromycin, third-generation cephalosporins or an extended duration of high-dose quinolone therapy should be considered for strains resistant to nalidixic acid or for patients who present from areas known to have a high rate of strains resistant to nalidixic acid.1,2
Returning to our patient, the Dominican Republic is considered an area of medium endemicity for typhoid fever. However, acquisition of typhoid fever at a 5-star resort is highly unusual, and there had been no reported outbreaks in this area. Our patient had no identified risk factors for typhoid fever, other than the use of a proton pump inhibitor, which can facilitate infection by decreasing gastric pH.1 The patient presented with typical clinical findings of mesenteric adenitis, but lacked other classic features of typhoid fever such as rose spots and relative bradycardia. The splenic infarct and subsequent hematoma may have arisen from intermittent atrial fibrillation with secondary bacterial seeding. This is a known complication1 but spontaneous splenic injury due to typhoid fever has also been reported.4
Our case demonstrates the potential difficulty in diagnosing typhoid fever, in part because of the relatively low sensitivity of blood, urine and stool cultures. The negative results of the bone marrow culture likely reflects the 14-day course of antibiotics. Testing for nalidixic acid resistance is important to determine fluoroquinolone resistance. In this case, the strain of S. typhi was sensitive to ciprofloxacin (according to established laboratory cutoffs); thus, the failure of ciprofloxacin therapy may have been the result of inadequate dosing. A higher dose of ciprofloxacin (20 mg/kg per day)1 may have prevented the recurrence.1
The prevention of typhoid fever rests heavily on education about food and water hygiene. Depending on the region of travel, vaccination may also be recomended. In particular, vaccination is recomended for people travelling to the Dominican Republic who plan to eat or drink outside major hotels. However, studies of oral and intramuscular/subcutaneous vaccines show incomplete protection (51% and 55% respectively).5
Footnotes
-
This article has been peer reviewed.
Competing interests: None declared.