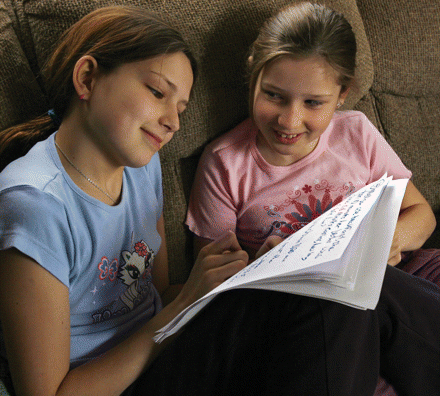- © 2007 Canadian Medical Association or its licensors
Should the vaccine against human papillomavirus be made available to young women and girls at public expense? Health Canada's National Advisory Committee on Immunization (NACI) and the Society of Obstetricians and Gynaecologists of Canada believe it should. But researchers, ethicists, and religious bodies have their doubts, raising questions about whether uncertainties surrounding the long-term efficacy of Gardasil (quadrivalent human papillomavirus types 6, 11, 16, 18, recombinant vaccine) justifies public funding, and whether vaccination programs will affect sexual behaviour.
Figure. The National Advisory Committee on Immunization is recommending that females aged 9–26 receive the new HPV vaccine. The question is, who will pay? Photo by: Canapress
The Merck Frosst vaccine, which costs $404 for 3 required doses, protects against HPV strains 16 and 18 that cause about 70% of cervical cancers, and strains 6 and 11 that cause 90% of genital warts (CMAJ 2006;175:234). It's projected that about 75% of sexually active Canadians will have at least 1 HPV infection in their lifetime, most of which resolve on their own. Some 1350 Canadian females are diagnosed with cervical cancer annually and about 390 die from it. (The NACI advises vaccinated females to continue having Pap smears.)
Gardasil was approved for sale in 2006 by Health Canada and in 55 other countries, including the US. Australia is publicly funding the vaccine for men and women. In some American states funding is available, and in others, debate rages. In Texas, for example, the governor is under pressure to rescind an executive order mandating that all grade 6 girls be vaccinated.
In mid-February, the NACI declared that Gardasil is safe and effective and should be delivered to girls aged 9–13 years (i.e., before the onset of sexual intercourse) and women between the ages of 14 and 26, even if they have had previous Pap smear abnormalities or HPV infections. That would mean vaccinating over 5 million females, at a cost of $2 billion for the vaccine alone. The NACI said the evidence was not clear enough to recommend that females over the age of 26, or males of any age, be vaccinated.
The recommendation is now in the hands of the Canadian Immunization Committee, which, for the first time, will coordinate federal–provincial–territorial discussions about implementation options and the cost-effectiveness of vaccine programs. Its report is not expected until late this year, and publicly funded programs are not expected for several years.
But some researchers say that the NACI's recommendations are premature because the science around the vaccine is evolving. Many issues, including how long Gardasil lasts and whether a booster will be required, remain unresolved. There is only 5 years worth of effectiveness data on Gardasil.
“I hope it actually confers long term immunity and protection, but at this point the evidence just isn't there,” says Ryan Melnychuk, a molecular virologist, ethicist and fellow in the Department of Bioethics at Dalhousie University. He also wonders whether some populations are more prone to infection or whether males should be vaccinated since Gardasil prevents genital warts.
Meanwhile, a second vaccine is in the works. GlaxoSmithKline's Cervarix will block HPV strains linked to 80% of cervical cancers — 10% more than Gardasil. But Cervarix, now in Phase 3 clinical trials involving Gardasil, does not target genital warts and the company hasn't yet revealed its price tag for the vaccine.
The question of cost-effectiveness looms large, but there are few studies weighing the relative cost-benefit ratios of the options. A background paper written for the BC Cancer Agency by economist and epidemiologist Hans Kreuger concluded that introducing Gardasil in BC in 2005 (assuming a cost of $330 and a booster at $100) would save $54 million in treatment costs over 26 years. But it would cost $373.6 million. “That's just saying we're avoiding the cost of treatment,” says Krueger. To break even at the end of 26 years, the vaccine would have to cost $45; a booster $15.
Dr. David McLean, head of the agency's Cancer Prevention Program, says health authorities need to explore cost-cutting strategies, including whether 2 shots, rather than 3, would “secure adequate coverage,” and whether focusing on subpopulations at higher risk (groups tending toward earlier sexual initiation or populations with higher cervical cancer rates) would be more cost-effective.
However, McLean cautions against using cost as the only measure of value. “Much of the expenditure in health could not in any way be termed cost-effective,” he says. “We do many things “because it is the right thing to do.”
Moreover, McLean notes evidence suggests that much oral cancer, cancers of the larynx and lung, and many skin cancers (combined with ultra violet light) are HPV related. “I think with a population program we may be very pleasantly surprised at what happens to the incidence of some other cancers.”
Still others have ethical issues with the vaccine. “I don't understand a mass vaccination for a sexually contracted disease,” says Moira McQueen, director of the Canadian Catholic Bioethics Institute at the University of Toronto. “It gives the clear message that we think sexual activity is okay at any age and they will be protected.” Education about the benefits of abstinence, she says, is a better long-term solution for emotional as well as physical health.
The debate will likely ratchet-up this year but NACI Chair Monika Naus doesn't believe it will be as intense as in the US. “I think that Canada is a lot more pragmatic about these kinds of issues,” she says. “I am sure there will be some controversy from some sectors, but I would hope that this would be seen as an opportunity rather than a hazard.”