A 43-year-old woman presented to the emergency department after 2 days of pain and swelling in her left thigh. She had no recent immobilization, trauma or surgery, nor a previous or family history of blood clots. She had been taking oral contraceptives for a month.
Examination showed her left thigh to be tender and 2 cm greater in circumference than her right. The results of blood tests, including a complete blood count, electrolytes, urea, creatinine, international normalized ratio (INR) and partial thromboplastin time, were within normal limits. Ultrasonography and CT investigations confirmed our diagnosis of deep-vein thrombosis with evidence of an extensive clot involving the left common and superficial femoral, left gonadal and left external iliac veins. She stopped taking the contraceptives and was prescribed dalteparin and warfarin. In clinic 4 days later, her leg pain had disappeared and the edema was resolving.
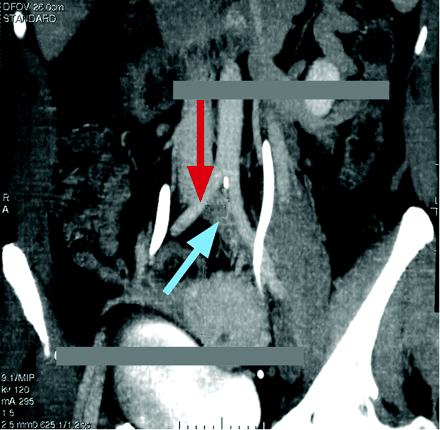
Two weeks later, she had recurrence of pain in her left leg and increased edema despite a therapeutic INR of 2.4. A repeat CT scan showed an iliofemoral clot with the same distribution as seen previously; marked narrowing of the left common iliac vein near its origin, however, constituted a new finding. Computerized 3-dimensional reconstruction revealed compression of the left common iliac vein by the right common iliac artery (Fig. 1on this scan image, the common iliac veins are indicated with blue arrows, and the arteries with red), a condition known as May– Thurner syndrome. A hypercoagulable work-up including tests for proteins C and S, factor V Leiden mutation, anti thrombin III, homocysteine, lupus anticoagulant, atiphospholipid antibodies and prothrombin G20210A proved noncontributory.
Our team placed a filter in the patient's inferior vena cava, did catheter-directed thrombolysis and put a stent in her left common iliac vein. Her symptoms resolved completely within 1 week and, at follow-up 14 months later, there was no recurrence.
In 1957, May and Thurner described an anatomic variant in which the left common iliac vein is compressed between the right common iliac artery and the lumbar vertebrae. This is considered a normal variant, with studies suggesting a prevalence of 25%–33% in the general population. Nonetheless, venous intimal hyperplasia from this compression may predispose one to stasis and clot formation. The term May– Thurner syndrome refers only to the minority of anatomic variants that declare themselves clinically. Left-sided venous stasis, edema, leg pain, varicosities and recurrent deep-vein thromboses have also been described, singly or in combination.1 May–Thurner syndrome accounts for up to 3% of all deep- vein thromboses. Women of reproductive age are at increased risk.
May–Thurner syndrome has greater morbidity than conventional deep-vein thrombosis. There is an up to 73% lifetime chance of recurrent thrombosis despite standard courses of anticoagulation.2 As many as 60% of patients with May– Thurner syndrome are predicted to have post-thrombotic syndrome (edema, pain, stasis dermatitis, ulcers or cellulitis) at some time during their lives.3 Catheter-directed thrombolysis with tissue plasminogen activator or urokinase appears to reduce the risk of post-thrombotic syndrome by one-half over 12 months, compared with conventional anticoagulation with warfarin (66% v. 33%, respectively). Stenting also has better outcomes than anticoagulation, with 87% vessel patency and symptom recurrence of only 20% at 41 months of follow-up.
May– Thurner syndrome should be considered in the diagnosis of patients who have isolated left-leg edema and venous insufficiency; left iliofemoral deep-vein thrombosis without a clear history of precipitants or an underlying clotting disorder; or left-sided symptoms that recur or persist despite adequate anticoagulation.