When Roy Romanow released his final report on medicare's future last November, he said home care was 1 of 5 key areas requiring national attention, and he called for a $1-billion transfer payment to kick-start the creation of a national home-care strategy. If this happens, Canadians can look east for a model, because New Brunswick now spends nearly 10% of its health budget on home care — double the provincial average.
New Brunswick's Extra-Mural Program, the “hospital without walls” concept that employs more than 640 full-time nurses and other professionals, provided care for almost 20 000 patients last year, including in-home acute, palliative and rehabilitative care. The service, launched in 1981 (CMAJ 1987;136:861-4), also helps coordinate support services and long-term care for mentally ill and elderly patients.
Physicians arrange admission to the program, prescribe treatment and order discharge, but in-home visits are the responsibility of the program staff. Depending on individual needs, staff may visit a patient as often as several times a day or as little as once a month.
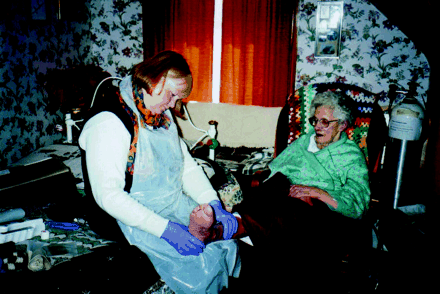
More than 70% of clients require nursing care. A typical day takes nurse Mary Anne McLellan over 100 km of highway and to the homes of up to 5 patients, where she deals with everything from wound care to IV therapy.
McLellan, who does her own case management and appreciates the autonomy she is given, says the program lets her “make decisions, and I am respected by physicians in those decisions.”
The province's physicians have come to rely on the assessment skills of the nurses, a survey conducted in southern New Brunswick indicates. Maureen McKee, director of that region's program, says many respondents indicated they would be at a loss without the program.
And being at home makes many patients feel more comfortable about asking questions. “The nurses are great for explaining my body systems,” one noted, “and they tell me what is happening, which is sometimes more than the doctors do.”
A palliative care patient's daughter, who is on leave from her job in Nova Scotia, wishes “the government of Nova Scotia would come across the border and see what sort of care is offered here. The program is wonderful.”
There has been no formal research on whether the program saves money, but Program Director Cheryl Hanson says it has eliminated the need for new hospital beds and the cost of maintaining them. More then 55% of patients admitted to the program are referred directly from the community, allowing them to avoid visits to the emergency room or admission to hospital.
Hanson thinks the NB program is an example of how home care can enhance medicare. “Home care is not only an option to be considered when beds are closing or when the hospital is experiencing a nursing shortage. Home health care is not cheap care and it is not second-class care — it is first-class care appropriate to the needs of the client and family.” — Tracey Thorne, Fredericton
Figure. RN Mary Anne McLellan with patient Photo by: Tracey Thorne