Canada's physician supply peaked in 1993 and has since dropped by 5% to 1987 levels, says a study by the Canadian Institute for Health Information (CIHI). But does this constitute an actual shortage?
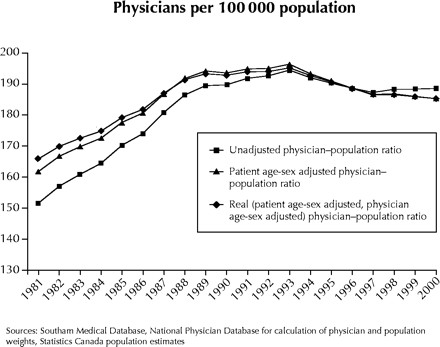
Figure.
The study, From Perceived Surplus to Perceived Shortage: What Happened to Canada's Physician Workforce in the 1990s?, was released June 6. It tracks physician–patient ratios over the last decade and examines the factors that created change, but author Ben Chan was careful not to describe the current situation as an “actual shortage” of physicians. Instead, he referred to it as a “shortage perception.”
He says society as a whole needs to think about the level of service it requires and is willing to pay for. Chan thinks the 1993 peak set expectations that have proven difficult to meet in subsequent years. Once MDs and their patients got used to the higher level of service available in 1993, their minimum expectations for care were set there and they had a hard time adjusting to a lower level of service. “A reduction of 5% is difficult for the population and providers to get used to.”
Chan, an MD and senior scientist at Toronto's Institute for Clinical Evaluative Sciences, says different policies contributed to current perceptions and realities. Some involved attempts to manage the physician supply, but policies on training, physician payment and spending controls may have had unintended consequences. The supply also diminished due to the increase in the number of elderly and female physicians — Chan says they tend to work less intensively — at the same time demand for services was increasing by 1.5% annually due to the growth and aging of the population.
Chan also says that one of Canada's most vilified physician supply measures — Morris Barer and Greg Stoddart's 1991 call for a 10% reduction in medical school enrolment — has received more blame than it deserves. “Much criticism and blame has been levelled at the 10% reduction, a direct policy intended to reduce physician supply,” states the CIHI study. Yet it finds that this policy accounted for no more than 2% of the overall decline in physician numbers in the 1990s: even though the move was implemented in 1993, the impact was only beginning to be felt in 1999. Chan says its full effect will emerge over the next decade. Overall, he found that enrolment cuts account for 11% of the decline in physician numbers in the 1990s, but this was largely due to enrolment cuts made in the 1980s, well before Barer and Stoddart arrived on the scene.
The biggest factor behind the drop in physician supply, accounting for 25% of the decline, is the increased time new doctors are spending in postgraduate training. “I was quite surprised by this result,” says Chan.
So was Dr. Hugh Scully, cochair of the Canadian Medical Forum's Task Force II on physician supply strategy. Scully says a few of Canada's 52 medical training programs have increased in length, but “it's hard to understand that this is the major effect. I don't buy it.”
But, according to the CIHI report, the elimination of the rotating internship effectively removed 1 year's worth of GPs from the market. After 1993, doctors wanting to practise family medicine needed 2 years of training after graduation, not 1. At the same time, a lot more graduates started opting for specialty training, which usually takes far longer than family medicine training.
“One area where we see a real decline is in the number of young family physicians,” says Chan. In the early 1990s, almost 80% of physicians started practice as FPs or GPs. By 2000, this percentage had plummeted to 45% (see CMAJ 166[11]:1449).
The study says another 22% of the decline occurred because fewer foreign doctors are coming to Canada due to policy changes, including visa restrictions, and there was also a 17% increase in the retirement rate. Although it has received a lot of press coverage, the brain-drain to the US and other countries accounted for only 3% of the decline.
Chan says he was struck by the speed at which the health care environ- ment changes. Canada now tends to do human-resource planning on an irregular 8-to-10-year cycle. “We need to plan on a yearly basis,” says Chan, “so we can respond much more quickly. We can't predict the future but we need to smooth the ups and downs that we face.”
The report used data from sources such as the Southam Medical Database, the National Physician Database and the College of Family Physicians of Canada's 2001 Janus Survey. — Steve Wharry and Barbara Sibbald, CMAJ










