The first artificial corneas based on human cells have been created by a team of scientists from Canada and the United States, bringing the production of artificial corneas suitable for transplant a significant step closer to reality.
Using as building blocks cells from the 3 layers of actual human corneas, Dr. May Griffith and colleagues from the University of Ottawa Eye Institute - in collaboration with scientists at Université Laval, University of Tennessee and the Procter and Gamble Company - engineered "corneal equivalents" that look and behave in lab tests very much like their natural counterparts (Science 1999;286:2169-72, see figure).
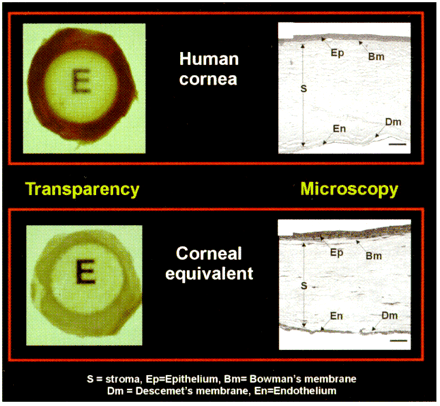
Figure. Comparison of corneal equivalent to human cornea.
The researchers began by isolating, then keeping alive, cells from the different corneal layers. Using these cells, they constructed the artificial corneas layer by layer around a "cellular scaffolding" structure. To produce a limitless supply of corneal cells for future research, the scientists also introduced viral genes to a few cells, causing them to multiply indefinitely.
While not yet ready for use in human transplants, the corneal equivalents developed through this tissue engineering method could soon put an end to using live animals' eyes to test the toxicity of new drugs and chemicals. The next step here is to develop a standard blueprint for the process, to ensure that its results can be repeated in other labs.
"We demonstrated that it is possible to reconstruct full-thickness corneas that have key morphological and functional properties of natural corneas," says Dr. Griffith, an assistant professor at the Eye Institute. "It is therefore possible to construct more 'natural' tissues that in the future may be useful for transplantation."
Dr. Griffith and her fellow researchers began the 5-year project in search of a workable model for research on healing damaged corneas. Because of high demand at human eye banks for transplant corneas, few are available for research purposes.
Artificial corneas could eventually meet growing demand for transplantation into people with diseased or injured corneas. Some experts predict a shortage in the supply of suitable corneas, based on an aging population and increased numbers of people having refractive laser surgery. The corrective procedure changes the shape and potentially the strength of corneas, rendering them unsuitable for harvest from postmortem donors.
Griffith says it is too early to speculate on when tissue engineering will yield transplant-ready corneas. "The real cornea is tough," said Griffith. "While our cornea looks and functions like real corneas, they do not yet have the toughness required for use in implants."