Results from the CMA's 1999 Physician Resource Questionnaire (PRQ) indicate that onerous on-call duty and other problems are taking a heavy toll on Canada's physicians.
One troubling sign that career burnout is becoming a serious problem was found in verbatim comments supplied by many of the more than 3100 respondents. "I have been off on a medical leave of absence this winter due to exhaustion," wrote one.
"Perhaps I am burnt out," added another. "I frequently feel sad that I became a physician. I want to retire as soon as possible."
So why are Canada's doctors so tired? A year ago, the PRQ found that more than one-third of physicians with on-call responsibilities considered these duties too demanding. In 1999, the PRQ attempted to delve into this issue by asking physicians to rate the level of stress associated with several aspects of on-call work. The results reported here, based on a 40.5% response rate from 8000 CMA members and nonmembers, are considered accurate within ± 1.8%, 19 times out of 20.
The most significant finding was that, measured on a 4-point scale, 57% of physicians who take call report that the lifestyle restrictions it imposes are stressful or highly stressful. Younger physicians who take call are more likely to be affected, with 65% of respondents under age 35 and 62% of those aged 35-44 stating that call-related lifestyle problems are stressful or highly stressful. Since these ages coincide with the prime child-rearing years, it is likely that call-based stress affects physicians' family life. "On call is the hardest part of the job," wrote one doctor. "Leaving my family at night and weekends without sufficient remuneration to take other time off is the hardest part of being a mom."
Her statement underscores another survey finding: only one-third of physicians who take call receive their preferred method of payment for providing these services. Although 71% of physicians receive only fee-for-service payments for call duties, this payment method is preferred by only 22% of them. A majority of physicians (55%) want on-call pay that is based on a sessional/hourly rate plus fee-for-service payments, but only 7% of doctors who take call are actually paid this way.
Verbatim comments suggest that on-call duties are difficult and financially frustrating. "Either there is compensation for on-call [work] so that we can see fewer patients in the office during the on-call week," one doctor complained, "or the call system will collapse completely."
There has been only a slight shift away from pure fee-for-service remuneration during the past decade. In 1990, 68% of physicians received 90% or more of their professional earnings from fee-for-service payments; by 1999, that proportion had dropped to 62%. However, there has been a large shift in the way physicians would prefer to be paid. Only 33% of respondents selected fee-for-service as their preference in 1999, compared with 50% in 1995. "As a new physician in fee-for-service, I find the weight of my practice responsibilities crushing," one physician explained. "I have student loans to pay, a business loan to pay, computer equipment in the office to buy. I feel burnt out, financially unable to take a vacation, and I have considered leaving medicine altogether. Please help us! A salary with benefits is how we deserve to be paid."
A substantial number of physicians (36%) reported a decrease in their net income in the 1999 PRQ, while 17.4% reported increased net income. Although the proportion experiencing a decline is lower than in 1998 (43%) and 1997 (50%), it still points toward a trend that angers many physicians. "I can't imagine doing this until I'm 65 years old, as expenses continue to rise more quickly than my wage increases," complained one doctor. "Soon it won't be worth working." FIGURE
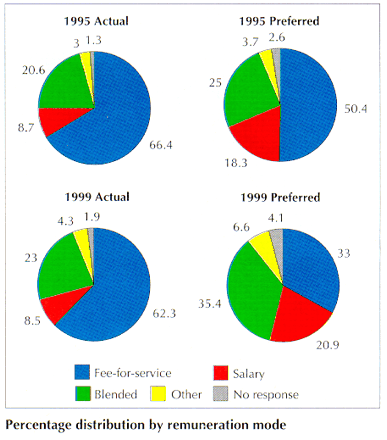
Figure. Percentage distribution by remuneration mode
Surgical specialists appear to be more susceptible to decreases in net income (44%) than GP/FPs (38%) and medical specialists (29%). Female doctors were notably less likely to report decreased income (30%) than were males (38%), and more likely to report increased income (21% vs. 16%).
Decreases in net income are not accompanied by decreases in hours worked; in fact, total hours of work have risen slightly in the past year, from 53.4 hours to 54.1 hours per week. Surgical specialists continue to put in the longest hours (58.7 hours/week) and female physicians spend fewer hours at work (49.4) than their male counterparts (56.2). More than half of all respondents (56%) saw their workload increase in the past 12 months; for females, the figure was 61%. Of those who said their workload increased in the past year, 32% experienced a decrease in net income. Slightly more than half of respondents (51%) who reported decreased net income also reported increased workloads.
Women with children under 18 at home worked fewer hours per week (46.6) than did those with no children (52.8). Men with children under age 18 at home worked more hours per week (58.1) than did those with no children (53.9). Women whose youngest child was under age 6 worked, on average, 43.9 hours per week, while men with very young children worked 57.5 hours per week.
Who cares for the kids?
For the first time since 1993, the PRQ gathered information about weekly hours spent taking primary responsibility for children and maintaining households. Male physicians spent less time on household maintenance, putting in an average of 7.9 hours/week versus 13.6 hours/week for female doctors. Female physicians reported spending an average of 41.1 hours/week with primary responsibility for children under age 18, a figure that is more than 3 times that reported by male physicians (12.2 hours/week).
Given these disparities, it is not surprising that female doctors tend to spend fewer hours per week on professional activities than their male colleagues. As is true for working women in general, female physicians are clearly responsible for what sociologist Arlie Hochschild calls "the second shift"1 - the long hours of family and household responsibilities that must be attended to before or after the workday. Reconciling the demands of the job with those of the second shift is not easy. "[It is] impossible for a female GP to run a practice, a viable business, and raise children with good values," a female physician commented. "I predict that more females will not practise in a GP setting."
The CMA conducted its first PRQ in 1982 and has been conducting them annually since 1997. It considers them a crucial long-term planning tool for the medical profession because they allow the association to track changes in physicians' attitudes and work practices.
Acknowledgments
Respondents who complete the CMA's Physician Resource Questionnaire, which is the largest of its type in the country, are invited to offer verbatim comments on medicine and their careers. In 1999, they had a lot to say.
-
"If I had to do it again, I'd never be a doctor - the responsibilities outside of home start on the day of graduation and never lighten until retirement or death."
-
"I'm a great believer in Canadian medicine and its positives, including a reasonable fee schedule (for nonsurgical procedures) and accounts receivable that are 99% good and paid promptly."
-
"We live in a small community, with our local hospital 15 km away. Two years ago we lost 4 family physicians, leaving us with 5. If we do not get more physicians or some respite from the responsibility, either stress or death will take 2 more of us."
-
"As the only neurologist from 1975 to 1978, I was on call 7 days a week for 3 years. The younger physicians are no longer willing to sacrifice the family life for the sake of on call."
-
"I work on salary for a native band that is delighted to have me and covers all office expenses. My overhead has virtually disappeared, the stress level is far lower and I get 9 weeks of paid leave, including 4 for education."
-
"With further deterioration of health resources, practice is less rewarding both economically and professionally. This will lead to my retirement as soon as possible, which will leave my community without primary care services."
-
"Is everyone as tired as I am?"
-
"I'm certain we take much better care of our patients than anyone takes care of us."
-
"We have lost 6 out of 19 physicians [FPs] since January, which has had a major impact on our workload and on-call commitments."
-
"Due to burnout and unforeseen family circumstances, I have gone from full time to less than 1 day per week in the last 18 months."
-
"I'm 40 years old. I really like what I do, but I think I am burned out. Maybe I'll move south."
-
"Prior to having 3 children in 3 years, I worked on average between 50-70 hours per week. I have worked less with each subsequent child. My main role now is as parent to my children, and I cannot help but feel a very strong discrimination against my choice."
Reference
- 1.↵










