Violence in the emergency department
FIGURE 1 Christopher Fernandes and colleagues surveyed emergency department employees working at a hospital in downtown Vancouver in 1996 to obtain estimates of the extent and effects of violence in their workplace. Ninety percent of the 106 respondents reported experiencing verbal abuse at least once a week, and 57% reported experiencing physical assault in 1996. The occupations with the highest proportion of respondents experiencing physical assault were nurses and protection services personnel. As a result of violence in the emergency department 73% reported some fear of patients and 38% had considered a job outside of health care. Because victims sought support most often from colleagues, the acquisition of debriefing skills by emergency department staff is recommended. In an accompanying editorial Laurie Morrison considers strategies to dowse this "emotional fire."
Figure 1.
See pages 1245 and 1262
Paramedic response to DNR requests
FIGURE 2 Ontario paramedics are bound by a duty to initiate aggressive life-support measures when responding to 9-1-1 cardiac arrest calls; however, this duty may conflict with the expressed wishes of patients with terminal illnesses. Veena Guru and colleagues reviewed the ambulance call reports of 144 terminally ill patients who were experiencing cardiac arrest. In 34 of those cases paramedics did not follow the regulations mandating resuscitation; although the presence (90 [62.5%] of the 144 patients) or absence of a do-not-resuscitate (DNR) request did not appear to influence the decision to resuscitate, paramedics were more likely to withhold full advanced cardiac life support in the presence of a DNR request. In their commentary Grant Innes and Karen Wanger find fault with physicians who fail to educate patients and their families about these issues and discuss the policy of the British Columbia Ambulance Service to honour a valid DNR form.

Figure 2.
See pages 1251 and 1264
Intraoperative MRI: a moving magnet
FIGURE 3 Magnetic resonance imaging (MRI) scanners generate exquisitely detailed images of the anatomy and pathology of the brain and spinal cord. Garnette Sutherland and Deon Louw describe the advent of intraoperative MRI scanners and the potential for minimalist surgery with maximum technical outcome. Although expensive ($2-3 million), costs can be offset by using the equipment for conventional diagnostic imaging when it is not required in the neurosurgical operating room. The authors predict that within a decade intraoperative MRI will become the standard of care in neurosurgery.
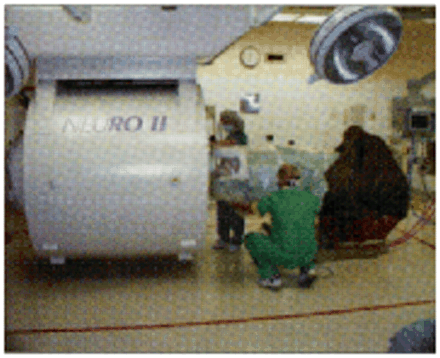
Figure 3.
See page 1293
Statins and myopathy
The incidence of muscle disorders (e.g., myopathy and rhabdomyolysis) can increase 10-fold when statins are combined with certain other drugs. Robert Herman provides a helpful review of the literature and the pharmacology of statins. Caution is warranted with lovastatin and simvastatin in particular because of their propensity toward a marked elevation in concentration if they are taken with a drug that inhibits first-pass metabolism. Lori Shapiro and Neil Shear discuss the role of the prescribing physician in detecting and reporting drug interactions and toxicities.
See pages 1281 and 1266
Footnotes
-
November 16, 1999










