Abstract
Background: Rates of death from cardiovascular and cerebrovascular diseases have been steadily declining over the past few decades. Whether such declines are occurring to a similar degree for common disorders such as acute myocardial infarction, heart failure and stroke is uncertain. We examined recent national trends in mortality and rates of hospital admission for these 3 conditions.
Methods: We analyzed mortality data from Statistic Canada’s Canadian Mortality Database and data on hospital admissions from the Canadian Institute for Health Information’s Hospital Morbidity Database for the period 1994–2004. We determined age- and sex-standardized rates of death and hospital admissions per 100 000 population aged 20 years and over as well as in-hospital case-fatality rates.
Results: The overall age- and sex-standardized rate of death from cardiovascular disease in Canada declined 30.0%, from 360.6 per 100 000 in 1994 to 252.5 per 100 000 in 2004. During the same period, the rate fell 38.1% for acute myocardial infarction, 23.5% for heart failure and 28.2% for stroke, with improvements observed across most age and sex groups. The age- and sex-standardized rate of hospital admissions decreased 27.6% for stroke and 27.2% for heart failure. The rate for acute myocardial infarction fell only 9.2%. In contrast, the relative decline in the inhospital case-fatality rate was greatest for acute myocardial infarction (33.1%; p < 0.001). Much smaller relative improvements in case-fatality rates were noted for heart failure (8.1%) and stroke (8.9%).
Interpretation: The rates of death and hospital admissions for acute myocardial infarction, heart failure and stroke in Canada changed at different rates over the 10-year study period. Awareness of these trends may guide future efforts for health promotion and health care planning and help to determine priorities for research and treatment.
See related commentary by Capewell and O’Flaherty, page 1283
Cardiovascular disease, including stroke, is the leading cause of death globally. Therefore, changes in the incidence and mortality of these disorders have a major impact on the overall health of a country’s population and on the health care system. 1 Rates of death from cardiovascular and cerebrovascular disease have been steadily declining in Western Europe and North America for the past 3 decades. 2,3 Whether this decline is occurring to a similar degree for common conditions such as acute myocardial infarction, heart failure and stroke is uncertain. Although these 3 conditions are associated with several common risk factors, the relative importance of risk factors such as smoking, hypertension and hyperlipidemia differs between them. 4 Furthermore, the rate of new therapeutic advances for these conditions has varied in both the acute, in-hospital setting and in the outpatient setting, where primary and secondary prevention of events occurs.
A comparative evaluation of recent population-based trends in incidence and mortality would provide an assessment of the relative progress achieved in preventing and treating these important conditions. Furthermore, the substantial economic impact of cardiovascular disease, including stroke, on the health care system — estimated at $18 billion per year in direct and indirect costs in Canada in 1998 5 — underscores the need for continued monitoring of cardiovascular disease and treatment outcomes. A study of temporal trends could also help guide future health promotion activities and health care planning.
We conducted a study of recent trends in the rates of death and hospital admissions for acute myocardial infarction, heart failure and stroke in Canada from 1994 to 2004. We also studied whether changes in these trends occurred at similar rates in younger and older Canadians and in both sexes.
Methods
Data collection
Mortality data
We obtained data on deaths from Jan. 1, 1994, to Dec. 31, 2004, from the Canadian Mortality Database, Statistics Canada’s national administrative death registry. This database receives information annually from all provincial and territorial registries of vital statistics on the cause of all deaths. 6 We used International Classification of Diseases (ICD) codes from the ninth and tenth revisions 7,8 to identify deaths for which the most responsible cause was cardiovascular disease. We used the ICD-10 codes because Canada switched from the ICD-9 to the ICD-10 coding system in 2000 for the coding of death certificates. We classified cardiovascular deaths overall and specifically for acute myocardial infarction, heart failure and stroke using the ICD-9 and ICD-10 codes shown in Appendix 1 (available at www.cmaj.ca/cgi/content/full/cmaj.081197/DC3). ICD codes for stroke are considered part of the overall category of cardiovascular disease; thus, our discussions of trends in the rates of death and hospital admissions for cardiovascular disease include stroke.
We determined the overall crude population-based rate of death per 100 000 population aged 20 years and over for each year by dividing the number of deaths for each condition by the size of the corresponding Canadian population, as determined from the Canadian census. In addition, we calculated the age- and sex-standardized rate of death through direct standardization to the 1991 Canadian population, the standard reference population recommended by Health Canada for disease surveillance. 9 We also calculated the rates of death for 4 age groups (20–49 years, 50–64, 65–74, and 75 and older) and for men and women.
Hospital admission and in-hospital case-fatality data
We determined the rates of hospital admissions from Apr. 1, 1994, to Mar. 31, 2004, because of acute myocardial infarction, heart failure and stroke using codes for the most responsible diagnosis (that which contributed the most to a patient’s length of stay) recorded in the Canadian Institute for Health Information’s Hospital Morbidity Database. We used the ICD-9 and ICD-10 codes shown in Appendix 1 (available at www.cmaj.ca/cgi/content/full/cmaj.081197/DC3) to classify the hospital admissions by condition. Previous studies have confirmed the high accuracy rate of coding of cardiovascular diseases and stroke in these databases. 10–14
To avoid double-counting of transferred patients, we created episodes of care whereby patients with the same encrypted health card number who were discharged from one institution and then admitted to another on the same day were assumed to have been transferred. We counted these patients only once. We calculated crude as well as age- and sex-standardized rates of hospital admissions per 100 000 population aged 20 and over. We also calculated crude, age- and sex-adjusted inhospital case-fatality rates based on episodes of care among patients admitted with these conditions over this period.
Statistical analysis
We determined 95% confidence intervals (CIs) for the rates of death and hospital admissions and in-hospital case-fatality rates using statistical boot-strapping techniques. We selected a random sample of patients from the study cohort of the same size as the original study cohort. Each patient could be selected once, multiple times, or not at all in the random sample. We then calculated the corresponding rates (e.g., rates of death) using the sample data set. After repeating the process 1000 times, the 95% CIs of the boot-strapped samples were obtained from the 2.5th and the 97.5th percentiles of the 1000 re-estimated rates.
Ethical approval
The study was approved by the research ethics board at the Sunnybrook Health Sciences Centre.
Results
Mortality
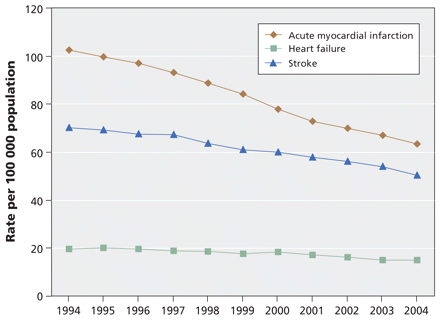
The overall trends in the rates of death for acute myocardial infarction, heart failure and stroke are shown in Table 1 and Figure 1. The population of Canada increased 14.4%, from 21 million people aged 20 and over in 1994 to 24 million in 2004. The all-cause mortality in Canada decreased from 933.1 per 100 000 in 1994 to 792.4 in 2004, a relative decline of 15.1% (95% CI 14.6%–15.5%). The overall age- and sex-standardized rate of death from cardiovascular disease declined 30.0% (95% CI 29.2%–30.7%), from 360.6 per 100 000 population aged 20 and over in 1994 to 252.5 per 100 000 in 2004. This represents an average annual rate of decline of 2.7%. The greatest decline was observed for deaths from acute myocardial infarction, which fell 38.1% (95% CI 36.9%–39.3%). This drop accounted for about 70% of the overall decrease in the number of deaths from cardiovascular disease. The age- and sex-standardized rate of death decreased 28.2% (95% CI 26.6%–29.8%) for stroke and 23.5% (95% CI 20.3%–26.5%) for heart failure.
Table 1: Trends in the rates of death, hospital admissions and in-hospital case fatality associated with acute myocardial infarction, heart failure and stroke in Canada, 1994–2004
Figure 1: Age- and sex-standardized rates of death from acute myocardial infarction, heart failure and stroke per 100 000 population aged 20 and over in Canada, 1994–2004. Rates are standardized to the Canadian 1991 census population.
Trends in mortality rates by age and sex groups are shown in Table 2. We observed decreases in the mortality rates for all 3 conditions in most age and sex groups. Historically, rates of death from cardiovascular disease in Canada have been higher among men than among women. In 1994, men represented slightly more than half (50.7%) of all cardiovascular deaths in Canada. By 2000, however, more women than men had died of cardiovascular disease. By 2004, 50.5% of all cardiovascular deaths in Canada were occurring in women. For all 3 conditions, deaths occurred predominantly among people aged 75 and over regardless of their sex (Table 2), although many deaths from acute myocardial infarction also occurred in younger groups. More men than women died of acute myocardial infarction; the opposite was true for heart failure and stroke.
Table 2: Age- and sex-specific rates of death by cardiovascular disease per 100 000 population aged 20 and over in Canada, 1994–2004
Rates of hospital admission
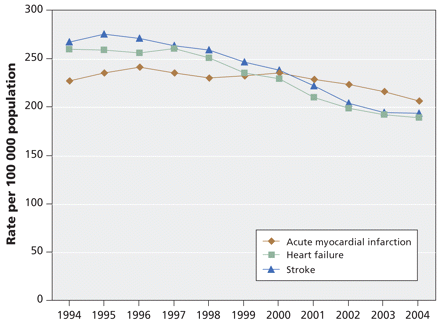
The overall rate of hospital admissions in Canada for any conditions declined 13.1% between 1995 and 2004. 15 The trend in hospital admissions because of heart failure and stroke declined steadily at similar rates, beginning in 1995 for stroke and in 1997 for heart failure (Figure 2). Overall, the rates of hospital admissions declined 27.2% (95% CI 26.3%–28.1%) for heart failure and 27.6% (95% CI 26.7%–28.4%) for stroke between 1994 and 2004 (Table 1).
Figure 2: Age- and sex-standardized rates of hospital admissions because of acute myocardial infarction, heart failure and stroke per 100 000 population aged 20 and over in Canada, 1994–2004. Rates are standardized to the Canadian 1991 census population.
In contrast, the rates for acute myocardial infarction were more varied. They declined from 1996 to 1998, increased in 1999, peaked in 2000 and declined modestly thereafter (Figure 2). The absolute number of hospital admissions because of acute myocardial infarction increased 16.1%, from 48 906 in 1994 to 56 759 in 2004, whereas the overall age- and sex-standardized rate declined 9.2% (95% CI 8.1%–10.3%).
We observed a shift in cardiovascular-related hospital admissions between 1994 and 2004 to an ever-increasing proportion of elderly patients for all 3 conditions (Table 3). In 2004, the median age of patients admitted because of acute myocardial infarction was 71, compared with 75 for those with stroke and 79 for those with heart failure. Men accounted for about two-thirds of all admissions because of acute myocardial infarction throughout the study period. The proportion of admissions because of heart failure and stroke remained similar between the 2 sexes. For all 3 conditions, women were more likely than men to be admitted to hospital at a later age, with a difference of 11 years for acute myocardial infarction and 5 years for both heart failure and stroke in 2004.
Table 3: Age- and sex-specific rates of hospital admissions by cardiovascular disease per 100 000 population aged 20 and over in Canada, 1994–2004
In-hospital case-fatality rates
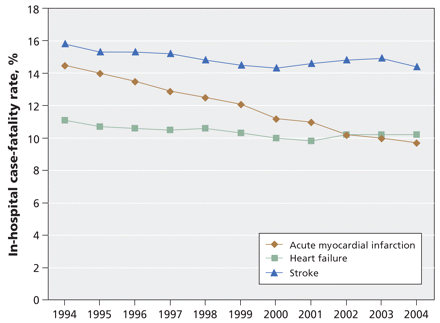
We observed a striking decline of 33.1% (95% CI 30.8%–35.6%) in the age- and sex-adjusted in-hospital case-fatality rate for acute myocardial infarction, from 14.5% in 1994 to 9.7% in 2004 (p < 0.001) (Table 1 and Figure 3). In contrast, more modest improvements were seen in the case-fatality rates for heart failure and stroke. The ratio of the number of patients who died during their hospital stay to the number who died of a cardiovascular cause as recorded on the death certificate was slightly less than one-third (Table 1). This suggested that much of the improvement in overall rates of death from cardiovascular disease were due to a decline in out-of-hospital deaths.
Figure 3: Age- and sex-adjusted in-hospital case-fatality rates among patients with acute myocardial infarction, heart failure and stroke in Canada, 1994–2004. Rates are standardized to the Canadian 1991 census population.
Interpretation
The decade of 1994 to 2004 was one of considerable investment and improvement in Canada in both the prevention and treatment of cardiovascular disease. We observed major reductions in all-cause mortality related to cardiovascular disease, including stroke, in Canada during this period, with an average annual rate of decline of about 3%. Similar annual rates of decline have been reported in the United States and in many Western European countries. 2,16 Much of the improvement in Canada was driven by declines in the rate of death from acute myocardial infarction, although the rates of death from heart failure and stroke also decreased significantly. In addition, we found increasing proportions of elderly Canadians being admitted to hospital because of cardiovascular disease and stroke and, for the first time, more women than men dying of cardiovascular disease. These data have important clinical and policy implications for practitioners and health system planners.
A key finding from our analysis was the rapid decline in the rate of death from acute myocardial infarction. Although it is not possible in Canada to distinguish out-of-hospital deaths from in-hospital deaths based on coding data from death certificates alone, we observed that about 4000 fewer Canadians died from acute myocardial infarction in 2004 than in 1994 despite a 16% increase in the absolute number of patients admitted to hospital because of acute myocardial infarction and a 14% increase in the size of the adult population in Canada. Our findings suggest that there were significant declines in the number of out-of-hospital deaths from acute myocardial infarction. This improvement could reflect declines in key risk factors for myocardial infarction, such as a reduction in the proportion of people in Canada aged 15 and over who smoke from 25% in 1999 to 20% in 2004, and better control of lipid levels and associated coronary plaque stabilization through increasing rates of statin use in Canada. 17,18
We also noted that the rate of hospital admissions because of acute myocardial infarction appeared to be declining between 1996 and 1998 but then rose again to a plateau in 2000 followed by a modest decline thereafter. The period from 1998 to 2000 coincided with the introduction of highly sensitive cardiac troponin assays in Canadian hospitals and a change in the European Society of Cardiology/American College of Cardiology epidemiological definition of myocardial infarction in 2000; 19 these changes probably resulted in some patients being classified as having an acute myocardial infarction whereas previously they would have been classified as having unstable angina. We observed striking and steady declines in the in-hospital case-fatality rates for acute myocardial infarction in both the pre- and post-troponin eras. These improvements probably reflect advances in treatment such as increased rates and timeliness of reperfusion therapy with primary angioplasty and fibrinolytic therapy along with increased use of acetylsalicylic acid, clopidogrel, β-blockers, angiotensin-converting-enzyme (ACE) inhibitors, angiotensin-receptor blockers and statins during the acute phase of myocardial infarction treatment, as has also been observed in other countries. 20
In contrast to acute myocardial infarction, the in-hospital case-fatality rate for stroke did not improve as much, although overall rates of death and hospital admissions because of stroke did decline significantly. Hypertension is the most important risk factor for stroke. During our study period, there were substantial increases in the use of antihypertensive medications such as diuretics, β-blockers, ACE inhibitors, angiotensin-receptor blockers and calcium-channel blockers in outpatients in Canada, along with the development of the Canadian Hypertension Education Program and better rates of hypertension control, as demonstrated in the Ontario Blood Pressure Prevalence Survey. 18,21 A major advance in the in-hospital treatment of stroke during this period was the use of thrombolytic therapy for ischemic stroke. However, only a small proportion of all stroke patients receive thrombolytic therapy, the major benefit of which is improvement in functional status rather than a reduction in in-hospital mortality. 22
Some studies have suggested a potential epidemic of heart failure because of the increasing elderly population and an increasing number of people who survive acute myocardial infarction. 23 The rate of hospital admissions because of heart failure has been steadily increasing in the United States, as compared with the decline we observed in Canada over similar periods. 24 The reasons for this difference are unknown, but it could reflect in part a higher admission threshold for patients with heart failure in Canada, since inpatient bed resources are more limited and many beds were closed between 1994 and 2004.
Our finding that more women than men in Canada are dying of cardiovascular causes is noteworthy. Historically, cardiovascular disease was considered a problem of middle-aged men. Our analysis showed a high burden of death and hospital admission related to cardiovascular disease among elderly women. This highlights the need for increased investment in education and research on cardiovascular health and disease in women. Both the American Heart Association and the Heart and Stroke Foundation of Canada have started public education campaigns aimed at better informing women about the risk factors and symptoms of cardiovascular disease. 25,26
Limitations
Our study has important limitations. Few studies have validated the accuracy of codes for causes of death in death certificates in Canada. 27 Validation studies conducted by the Framingham study investigators in the United States have shown that death certificates may be miscoded and may not correspond with the cause of death found at autopsy. 28 Canada changed its coding system for death certificates from the ICD-9 to the ICD-10 coding system in 2000, which may have introduced a coding artifact. However, we did not detect any abrupt changes in the frequency of various causes of death after the introduction of the ICD-10 system, which suggests that this was not a major issue.
Another limitation was our inability to link the data on hospital admissions to the mortality data at a national level. Such a linkage would have enabled us to determine the exact proportion of in-hospital versus out-of-hospital deaths for all 3 conditions. It would have also allowed us to determine 30-day case-fatality rates in addition to in-hospital case-fatality rates, which potentially are influenced by changes in length of stay after a hospitalization.
A final limitation was our inability to determine what proportion of hospital admissions were new versus repeat admissions. Although changes in the rates of hospital admissions probably reflect changes in the underlying incidence rates of disease, the determination of the true incidence of new events would best be done through labor-intensive chart reviews of deaths and admissions. However, this would be difficult to conduct at a national level because of the costs involved as well as privacy restrictions on data access.
Conclusions
We observed significant declines in population-based rates of death and hospital admissions for acute myocardial infarction, heart failure and stroke in Canada from 1994 to 2004. However, these findings are not grounds for complacency. Cardiovascular disease continues to be the leading cause of death and reason for hospital admissions in Canada. Our findings suggest that previous efforts to prevent cardiovascular events have been successful, but in many cases they may have delayed the occurrence of such events until people are older and potentially more difficult to treat. Further advances in prevention and treatment are required along with continued nationwide surveillance of cardiovascular events. The declines in mortality that we observed may plateau or even be reversed in the future because of increasing rates of key risk factors such as obesity and diabetes. 29 The recent development of a national Canadian Heart Health Strategy (www.chhs-scsc.ca/web/) may serve to help facilitate coordinated efforts to reduce the burden of cardiovascular disease on the health of Canadians and the health care system.
Footnotes
-
An abridged version of this article appeared in the June 23 issue of CMAJ
This article has been peer reviewed.
Competing interests: None declared.
Contributors: All of the authors contributed to the conception and design of the study, acquisition and interpretation of the data, and drafting and revising of the manuscript. All of the authors approved the final version submitted for publication.
Acknowledgements: We thank Tara O’Neill and Linda Donovan for their assistance in the preparation of this manuscript.
Parts of this material are based on data and information provided by the Canadian Institutes for Health Information. The analyses, conclusions, opinions and statements expressed are those of the authors and not necessarily those of the Canadian Institute for Health Information.
Funding: This study was supported by a Team Grant in Cardiovascular Outcomes Research to the Canadian Cardiovascular Outcomes Research Team (www.ccort.ca) from the Canadian Institutes of Health Research. Jack Tu is supported by a Canada Research Chair in Health Services Research, Ottawa, Ont., and by a Career Investigator Award from the Heart and Stroke Foundation of Ontario, Toronto, Ont.
The Institute for Clinical Evaluative Sciences is funded by an annual grant from the Ontario Ministry of Health and Long-Term Care. The opinions, results and conclusions reported in this paper are those of the authors and are independent from the funding sources. No endorsement by Institute for Clinical Evaluative Sciences or the Ontario Ministry of Health and Long-Term Care is intended or should be inferred.
The Canadian Cardiovascular Outcomes Research Team: Jack V. Tu MD MSc PhD, Institute for Clinical Evaluative Sciences, Sunnybrook Health Sciences Centre, University of Toronto; William Ghali MD MPH, University of Calgary; Louise Pilote MD MPH PhD, Division of General Internal Medicine, McGill University and McGill University Health Centre; Jafna L. Cox BA MD, Division of Cardiology, Dalhousie University, Capital Health; Douglas S. Lee MD PhD, Institute for Clinical Evaluative Sciences, Division of Cardiology, Toronto General Hospital; Karin H. Humphries MBA DSc, University of British Columbia, Division of Cardiology; David Alter MD PhD, Institute for Clinical Evaluative Sciences, Division of Cardiology, St. Michael’s Hospital and the Toronto Rehabilitation Institute; Peter C. Austin PhD, Institute for Clinical Evaluative Sciences, Dalla Lana School of Public Health, University of Toronto; Mark J. Eisenberg MD MPH, Divisions of Cardiology and Clinical Epidemiology Jewish General Hospital, McGill University; William M. Flanagan BM, Statistics Canada; P. Diane Galbraith BN MSc, Foothills Medical Centre, University of Calgary; Michelle M. Graham MD, University of Alberta; Ansar Hassan MD PhD, Department of Cardiac Surgery, Saint John Regional Hospital, Atlantic Health Sciences Corporation; Gregory M. Hirsch MD, Department of Surgery, Dalhousie University; Thao Huynh MD MSc, Research Institute of the McGill University Health Centre; Cynthia A. Jackevicius BScPhm PharmD MSc, Western University of Health Sciences, Institute for Clinical Evaluative Sciences; Helen L. Johansen PhD, Health Analysis Division, Statistics Canada, Department of Community Medicine and Epidemiology, University of Ottawa; Merril L. Knudtson MD, Libin Cardiovascular Institute of Alberta; Dennis T. Ko MD MSc, Division of Cardiology, Schulich Heart Centre, Sunnybrook Health Sciences Centre, University of Toronto, Institute for Clinical Evaluative Sciences; Michael P. Love MB ChB MD, Department of Medicine, Queen Elizabeth II Health Sciences Centre, Dalhousie University; Doug Manuel MD MSc, Ottawa Health Research Institute; Colleen M. Norris, RN PhD (Epid), Faculties of Nursing and Medicine, University of Alberta; Wayne Putnam MD, Department of Family Medicine, Dalhousie University; Stéphane Rinfret MD SM, Institut Universitaire de Cardiologie et de Pneumologie de Québec, Université Laval; Michael J. Schull MD MSc, Institute for Clinical Evaluative Sciences, Department of Medicine, University of Toronto; Derek Y. So MD, University of Ottawa Heart Institute; Therese A. Stukel PhD, Institute for Clinical Evaluative Sciences; Lawrence W. Svenson BGS DipPsych, Surveillance and Environmental Health, Alberta Health and Wellness, School of Public Health, University of Alberta; Christopher R. Thompson MD CM, St. Paul’s Hospital, University of British Columbia; Karen Tu MD MSc, Institute for Clinical Evaluative Sciences, Department of Family and Community Medicine, University of Toronto; and Nancy A. Walton PhD, Daphne Cockwell School of Nursing Chair, Research Ethics Board, Ryerson University.
Additional graphs and PowerPoint slides of data from this study are available for presentations at www.ccort.ca/Trends.aspx.