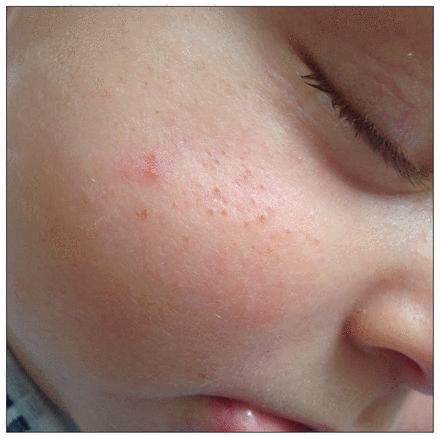
A previously healthy four-month-old boy presented with a one-month history of recurrent pustules, erythematous nodules and comedones on his cheeks. Physical examination did not show any signs of virilization. Based on the child’s age and lesion morphology, a diagnosis of infantile acne was made. After discussion with the family, an expectant approach was agreed upon.
Pediatric acne can be divided into five subgroups: neonatal, infantile, midchildhood, preadolescent and adolescent. Neonatal acne is common, affecting 20% of infants younger than six weeks.1 It is an inflammatory response to the saprophytic yeast Malassezia and is not true acne.1 It presents with inflammatory papules and pustules, is more common in boys, resolves by four months of age and rarely requires treatment.1
Multiple comedones on the cheek of a four-month-old boy.
Infantile acne has a similar lesion distribution and male predominance but includes comedones, nodules and cysts. In rare instances in which infantile acne is severe and persistent, or when additional signs of virilization are noted, underlying endocrinopathies must be considered. 2,3 It presents later (age 3–16 mo) and is much less common, affecting less than 2% of children.2,3 Infantile acne may persist for one to two years and has been linked to an increased incidence and severity of adolescent acne.1
All cases of acne presenting in midchildhood (age one to seven years) should be investigated for hyperandrogenism.1,2,4
Unlike neonatal acne, infantile acne can result in scarring. The risk of scarring is difficult to estimate but increases with severity of acne and in patients with darker skin. Early and effective treatment of substantial infantile acne can reduce that risk.4
Topical treatments are effective in mild cases of infantile acne consisting of comedones and pustules and include benzoyl peroxide, retinoids, azelaic acid and antibiotics.3,4 Oral antibiotics (erythromycin or trimethoprim) or oral isotretinoin can be used for severe infantile acne involving deep nodules and cysts.3,4
Clinical images are chosen because they are particularly intriguing, classic or dramatic. Submissions of clear, appropriately labelled high-resolution images must be accompanied by a figure caption and the patient’s written consent for publication. A brief explanation (250 words maximum) of the educational significance of the images with minimal references is required.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.