Vancouver doctors looking for a more effective way to treat the life-threatening fungal infections of their HIV-positive, injection-drug–addicted patients prompted research into a drug that could also save the lives of patients with parasitic infections in the developing world.
And in a deal signed with the University of British Columbia in Vancouver, BC, the promising formulation for an oral dose of amphotericin B — which now has to be administered intravenously — will be developed under the institution’s global access principles.
The university is the first in Canada, and 1 of only 4 in North America, to have formally adopted such principles, under which it will provide licences to companies to develop research. In exchange for rights in the developed world, the firms must agree to make the resulting drug or device available at low cost to the developing world.
A “wave” of similar approaches is coming within the nation’s universities, said Angus Livingston, managing director of UBC’s university-industry liaison office.
None too soon, according to speakers at Universities, Innovation and Global Medicine Access, an Apr. 20–21 conference held at the University of Toronto’s Munk Centre for International Studies in Toronto, Ontario.
Fourteen million people a year (90% of those from developing countries) now die from infectious diseases, said Dr. James Orbinski, a fellow at the Munk Centre. But research and development activity into the diseases of the global south are at “a virtual standstill.”
The role of universities in addressing this humanitarian crisis was the main focus of the conference, cosponsored by the student group Universities Allied for Essential Medicines (CMAJ 2007;176[7]:914–15) and the Initiative for Drug Equity and Access at the University of Toronto’s faculty of pharmacy (http://phm.utoronto.ca/~idea).
“The knowledge economy is an innovation economy” and universities are a key source of innovation, said Lorna Jean Edwards, University of Toronto assistant vice-president of international relations.
As a result, universities have a specific role to “manage the deployment of our innovations for the public benefit … the moral imperative to act is clear,” states a letter signed by many conference attendees.
The global financial crisis, rising food costs and drastic cuts to global health funding and disease surveillance mean there’s a “brutal decade” ahead for the world’s poor, predicted Orbinski. The University of Toronto associate professor of medicine and former Médecins Sans Frontières president added that 6 of the United Nations’ 8 Millenium Development Goals, which were to be reached by 2015, are now set to fail.
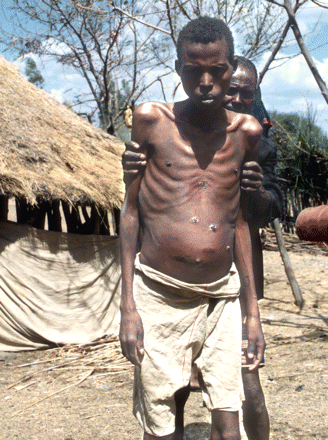
A patient seeking treatment in Arba Minch, Ethiopia is so weakened by visceral leishmaniasis that he needs support to stand and walk. His distended belly is caused by an enlarged spleen and liver. Image courtesy of Asrat Hailu / Leishmaniasis East Africa Platform
Improving the developing world’s access to life-saving drugs would help address needs, although Orbinski labelled as “rhetorical successes but practical failures” 2 efforts in that direction: Canada’s Access to Medicines Regime, and trade commitments made at a World Trade Organization meeting in Doha, Qatar, in 2001. Bilateral trade agreements have since rendered those commitments unattainable.
Meanwhile, new drugs are needed for a wide range of diseases that affect poor people. But it’s “not science that drives choices for scientific investigation,” Orbinski says. “It’s business values and return on investment. There are hundreds of promising compounds … that will never make it through the pipeline.”
That is where universities can play a role. “Scientists were so excited when we contacted them,” said Jana Armstrong, director of the Drugs for Neglected Diseases Initiative in North America. The organization developed partnerships such as the Malaria Vaccine Initiative and expects to have 6 to 8 new treatments for neglected diseases available by 2014. Among its activities is searching out promising compounds or alternative uses for existing drugs. As an example of the latter, UBC’s liaison office alerted pharmacy professor Kishor Wasan (who had been asked by Vancouver doctors to develop an oral form of amphotericin B) to the possiblility that the formulation could be used for visceral leishmaniasis, a fatal infection that attacks the spleen and the liver, and trypanosomiasis.
Meanwhile Wasan says his uncle —Mumbai, India, physician Dr. Pravin Khullar — reinforced the need to have an oral form of the drug available in villages, where sufferers don’t have ready access to intravenous treatment. “My uncle also says the WHO [World Health Organization] estimates of 1.5 million cases a year are far too low,” said Wasan, who was recently named Chair in Drug Delivery for Neglected Global Diseases, jointly sponsored at UBC by the Canadian Institutes of Health Research and the Vancouver biotechnology firm iCo Therapeutics Inc., which licensed his formulation.
University technology transfer offices are rethinking their role, and encouraging members to embrace global access principles, said Ashley Stevens, incoming president of the Deerfield, Illinois-based Association of University Technology Managers. That often involves engaging with international organizations such as the Bill and Melinda Gates Foundation and WHO.